Dear Editor,
Although surgical removal of the epiretinal membrane (ERM) in symptomatic patients is frequently performed and provides quite good anatomical and functional results, ERM peeling often causes complications such as cataract formation in phakic eyes, retinal tear or detachment, and macular edema [1]. Choroidal neovascularization (CNV) development after ERM removal is very rare, with only seven reported cases [2]. We encountered one case of iatrogenic CNV following vitrectomy for ERM peeling in which intravitreal af libercept injection resulted in successful CNV regression. We report this case with a literature review.
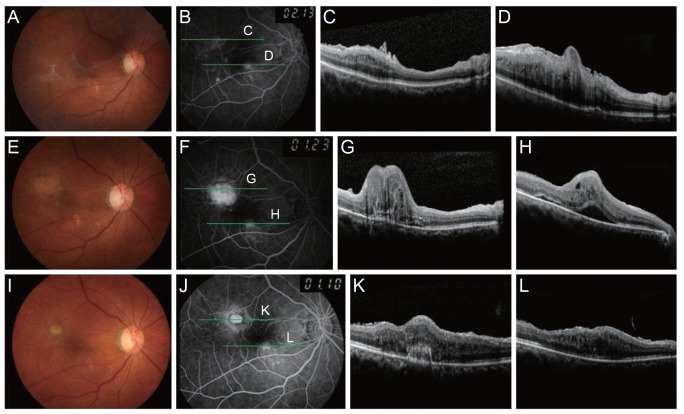
A 74-year-old woman presented with decreased vision and metamorphopsia of the right eye. The best-corrected visual acuity (BCVA) was 20 / 200 and 20 / 25 in the right and left eyes, respectively. She had previously undergone bilateral cataract surgery at another clinic. Fundus examination showed ERM in the right eye (Fig. 1A-1D). The patient underwent pars plana vitrectomy with membrane removal without intraoperative complications. Four weeks after surgery, the BCVA was 20 / 130 in her right eye, and the ERM was successfully removed. However, she still complained of blurred vision in the right eye. Extrafoveal CNV was found on fundus examination and was confirmed by fluorescein angiography and optical coherence tomography (Fig. 1E-1H). Given the diagnosis of CNV, intravitreal aflibercept (Eylea, Bayer Pharma AG, Berlin, Germany) injections were applied in the right eye three times at four-week intervals, and one more injection was administered two months after the third injection. At one year after surgery, the CNV had regressed without recurrence (Fig. 1I-1L), and the BCVA in the right eye had improved to 20 / 100.
The cause of CNV formation and its relationship to ERM removal have not been clearly elucidated. We propose that trauma during surgery, such as retinal pigment epithelium and Bruch's membrane disruption [3], is the most likely cause of CNV for several reasons. First, iatrogenic CNV secondary to ERM peeling usually develops in the extrafoveal region where the ERM was located, as observed in this patient and in other reported cases [2], while CNV associated with age-related macular degeneration is generally located under the foveal area. Second, CNV occurred within 1 month after operation in our case. However, preoperative subclinical changes related to early age-related macular degeneration might be another cause or risk factor of CNV development [3]. Preoperative fundus photographs demonstrated several macular drusen with pigmentary change in this patient.
CNV after ERM removal is treated similarly to CNV from other etiologies. Therapeutic options such as laser photocoagulation, intravitreal anti-vascular endothelial growth factor antibody injection, photodynamic therapy, or vitrectomy have been reported [2,3]. Mechanical injuries during ERM removal might induce the reparative process, including retinal pigment epithelium activation and vascular endothelial growth factor release, which similarly occur in CNV formation secondary to age-related macular degeneration [2]. In our case, repeated aflibercept injections resulted in successful CNV regression and improved vision. This is the first reported case treated with aflibercept for CNV after ERM peeling. However, no consensus regarding treatment strategies has been reached because of the limited number of cases. Further investigation with more patients and long-term follow-up is required.
In conclusion, secondary CNV is an uncommon complication following successful surgery for ERM. Surgeons should be aware of this complication, as timely diagnosis and treatment are required to prevent visual deterioration.



 PDF Links
PDF Links PubReader
PubReader Full text via DOI
Full text via DOI Full text via PMC
Full text via PMC Download Citation
Download Citation Print
Print






