 |
 |
| Korean J Ophthalmol > Volume 27(5); 2013 > Article |
Abstract
Purpose
To identify the unique pathologic findings of retinal angiomatous proliferation (RAP) in optical coherence tomography (OCT).
Methods
Retrospectively, 29 eyes of 25 patients with age-related macular degeneration and complicated RAP were analyzed. All 29 eyes had choroidal neovascularization (CNV) in the area of pigment epithelial detachment (PED) or adjacent to it, which was visible with fluorescein angiography or indocyanine green angiography. Cross-sectional images were obtained by OCT scanning through the CNV lesions.
Retinal angiomatous proliferation (RAP) refers to a neovascular form of age-related macular degeneration (ARMD) originating from the inner retinal vasculature [1]. It is characterized by peculiar hemorrhagic lesions accompanied by exudation and retinal microangiopathic changes in which is new vessels grow from the choroid called choroidal neovascularization (CNV) [2,3].
Recent studies have demonstrated histopathologic correlations that have expanded our knowledge regarding RAP. It is now evident that subretinal neovascularization in the posterior limits of the retina arises from retinal capillary proliferation or intraretinal neovascularization [4-7]. The process of neovascularization is often associated with the formation of a serous pigment epithelial detachment (PED) and CNV which may result in retinal-choroidal anastomosis (RCA) [4,5,8].
Fluorescein angiography (FA) has played a key role in understanding the pathophysiology of various presentations of ARMD [6,7]. However, more accurate diagnosis of RAP has been established with indocyanine green angiography (ICGA) which identifies neovascularization more accurately than FA, where an ill-defined area is seen in the intra- and subretinal vessels underlying the layer of sensory retina or retinal pigment epithelium detachment [4,9-11].
Spectral-domain (SD)-optical coherence tomography (OCT) is a noninvasive diagnostic method that provides high-resolution cross-sectional images of the retina and is a valuable tool for monitoring macular disease; yet, OCT has been used primarily as a complementary tool to FA and ICGA in the diagnosis RAP [6,7,12].
This study intends to elucidate the pathologic findings of RAP by OCT in terms and patterns which have not been depicted by previous studies. Furthermore, we attempt to propose characteristic findings of OCT in patients with RAP that may be diagnostically significant.
We studied 29 eyes of 25 patients with exudative ARMD complicated by RAP of variable onset that were identified from January, 2007 to January, 2011. The diagnosis of RAP was based on angiographic evidence (FA and ICGA) of an intraretinal neovascular complex connected with the retinal circulation, the patients were subjected to one of the three vasogenic stages described by Yannuzzi et al. [4] (stage I: intraretinal neovascularization, stage II: subretinal neovascularization with or without PED, and stage III: CNV with RCA). All patients were older than 53 years and exhibited unique presentations of ARMD, such as soft or exudative drusen, retinal pigment epithelium (RPE) pigmentation and geographic atrophy.
None of the patients had other neovascular maculopathy that may be complicated by chorio-retinal anastomosis, such as infectious or inflammatory chorioretinal disease, angioid streaks, hereditary retinal disorders or trauma. We performed a complete ophthalmologic examination including FA (Digital retinal camera CX-1; Canon, Tokyo, Japan), dynamic ICGA (HRA2-KT-02972; Heidelberg Engineering, Heidelberg, Germany) and OCT (Spectral OCT SLO; A Division of OPKO Health, Toronto, Canada) in all 29 eyes.
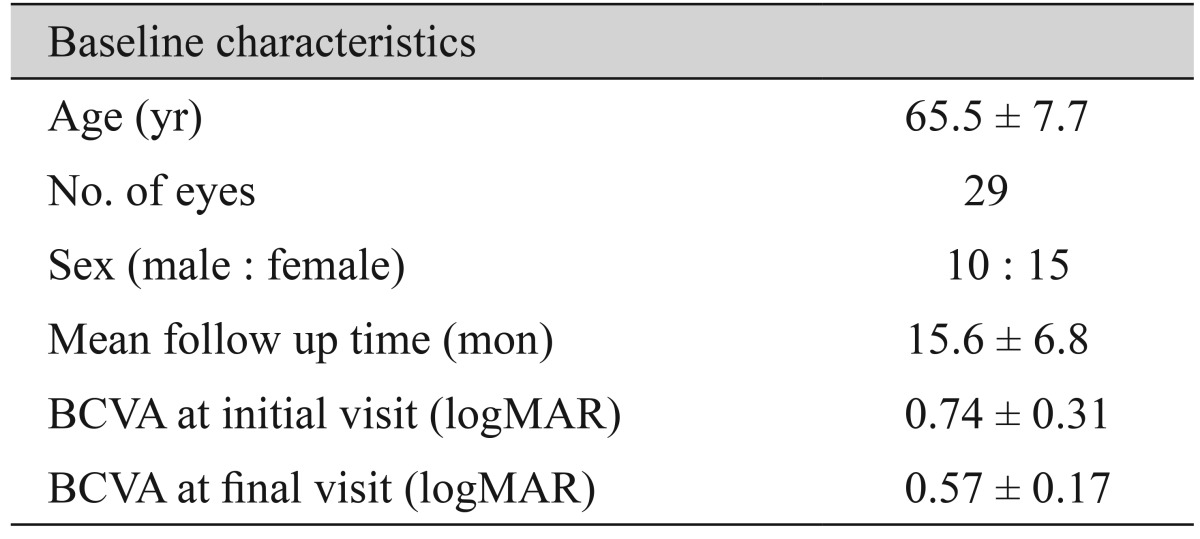
A total of 29 eyes of 25 patients diagnosed with RAP were examined in this study. The patients were all of Asian descent, including 10 (40%) men and 15 (60%) women. The mean age of the patients was 65.5 ± 7.7 years (range, 53 to 81 years). The best-corrected visual acuity (BCVA) of the patients at initial and final visits were 0.74 ± 0.31 and 0.57 ± 0.17, respectively (Table 1).
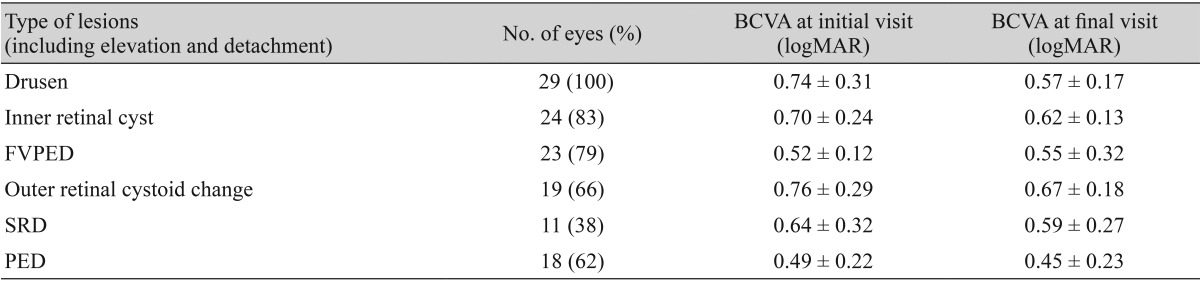
Based on the FA angiograms, all eyes demonstrated an ill-defined leakage which produced an indiscreet continuous zone within and beneath the retina. A hyperreflective focal area inside the neuroretinal layers, corresponding to the intraretinal vascular complex seen in FA and ICGA, was detected in all OCT scans. OCT revealed drusen in 29 eyes (100%); out of these 29 eyes, 24 eyes had inner retinal cyst. In 18 eyes the inner retinal cysts were accompanied by the outer retinal cystoid change, whereas in eight eyes there were no outer retinal cystoid changes. Fibrovascular pigment epithelium detachment (FVPED) which was observed in 23 eyes (79%), 18 of which also had outer retinal cystoids change. No patient had outer retinal cystoid change or subretinal detachment (SRD) without other accompanying findings. Of the 11 eyes evidencing SRD, all 11 also displayed FVPED, and nine eyes (82%) also had PED. BCVA at initial and final visit of each of the 6 groups according to the OCT findings were also analyzed (Table 2).
Drusen are formed by the deposition of lipofuscin (a type of retinal waste product) and by the separation of RPE from its underlying basement membrane [13]. Drusen are characterized by hyperreflective mounds beneath the RPE layer on OCT that, at large sizes, may displace retinal tissue. In our experience, drusen is present in 100% of cases previously diagnosed as RAP; yet it is almost always accompanied by the other findings observed in our study including elevation and detachment of different layers of retina (Fig. 1).
Inner retinal cyst formation is often present with cystoid macular edema and is represented by round, minimally reflective (darker) spaces within the neurosensory retina. Large cysts may be able to expand to the entire thickness of the retina from the retinal pigment epithelium/choriocapillaris (the anterior boundary of neurosensory retina). In this study, four of the patients were initially diagnosed with unilateral RAP but later on RAP developed in the fellow eyes. In these patients, the first common finding in eyes without RAP was inner retinal cysts, which were present even when CNV was not detected (Fig. 2).
Along with neovascularization, disruption of the normal outer retinal and inner choroidal anatomy result in fibrovascular proliferation along with the accumulation of fluid in the subretinal pigmented epithelium (sub-RPE) space, the subretinal space, and within the retina. In our study, 79% of the eyes with RAP showed FVPED accompanied by retinal and subretinal tissue thickening (Fig. 3).
Outer retinal cysts (ORCs) are cystic lesions confined to the retina's outer nuclear layer; they are usually located next to a pre-retinal fibrotic area or an area of retinal atrophy. FA reveals minute dots of fluorescence which correspond to leakages, typically in the late phase. In this study, a majority of the patients had cystoid changes in the outer retinal layer than ORCs where hyperreflective rings surrounding cystic cavities were absent on OCT when advanced. However, 66% of the patients demonstrated such alterations in the outer retinal layer which was sufficient to be considered meaningful (Fig. 4).
Subretinal fluid appears as a non-reflective (dark) space between the posterior boundary of the neurosensory retina and the retinal pigment epithelium/choriocapillaris reflection on OCT. Apart from intraretinal edema, the nonreflective area is not present within the neurosensory retina. The neurosensory retina overlaying the area of subretinal fluid is typically not thickened on OCT images except when the subretinal fluid has been chronic (Fig. 5).
Detached RPE is slightly more reflective where increased reflectivity of the RPE band severely shadows reflections from the choroid. Hemorrhagic RPE detachments are distinguished by a moderately reflective layer directly beneath the detached RPE. Fibrovascular RPE detachments demonstrate moderate reflectivity throughout the entire sub-RPE space. In this study, even in cases without clearly demonstrated CNV, PED on OCT were accompanied by FVPED and/or SRD in all patients, which implicates the presence of CNV at some level. CNV may have been masked by fluids, hemorrhages or space-occupying lesions (Fig. 6).
RAP has emerged as an increasingly acknowledged variant of neovascular ARMD [4,14-16]. Lesions of RAP originate from intraretinal neovascularization. Branches of new vessels extend into the subretinal space resulting in RPE detachments and anastomosis with choroidal neovascular complexes [17].
FA often results in angiographic presentations of occult or minimally classic CNV in patients with RAP. When large PED are presence, it had been difficult to reveal in RAP lesion by FA. CNV is known to originate from the choroid, then PED is formed and the fluid leaks into the retina [3]. However, RAP originates where leakage in the retina occurs, and PED is subsequently formed. This may be why it is difficult to detect the exact location where RAP lies with FA, especially in the earliest stages of the disease with PED in RAP lesions, due to the presence of intraretinal fluid [3,12,14].
ICGA is a useful tool in determining the nature of neovascularization, which appears as indistinct hyperfluorescence in FA, because it establishes the relationship between RAP and retinal circulation [3,10-12]. However, both FA and ICGA are tools that give us information by two dimension image. Rouvas et al. [3] employed Stratus OCT evaluation and revealed CNV with a small surface area beneath circular and irregular RAP lesions in focal or multifocal RAP, which provided better perspectives for understanding this disease. Thus, we believe that, investigating the non-CNV lesions that commonly accompany RAP lesions with spectral domain OCT may be helpful in the diagnosis and consideration of subsequent treatment. We investigated lesions that may occur alone or in combination in patients with RAP, and did so independently from the classification and staging proposed by Yannuzzi et al. [4] since the true nature of RAP lesions had not been clearly identified.
Drusen, hyperfluorescent, ill-defined confluent lesions on FA which are tiny yellow or white accumulations of extracellular material that build up in Bruch's membrane. The presence of a few small drusen is normal with advancing age (>40 years old), especially in patients with progressing ARMD [18-20]. Drusen are typically found easily in patients with RAP; this may not be a diagnostic finding; but it may be helpful in locating other lesions and which layers of they lie within, since drusen usually appear in combination with others findings including SRD and PED.
The biomicroscopic location of RAP lesion is difficult to assess because it is usually masked by intraretinal proliferations including edema and hemorrhages [2]. In the present study, intraretinal serous edema was commonly found in the presentation of inner retinal cyst together with FVPED. Inner retinal cysts are lesions typically accompanied by cavitation and the subsequent retinal swelling caused by accumulation of intraretinal fluid, and their layer of origin can be difficult to detect FA and/or ICGA [6,7-9].
Although OCT is an excellent tool for diagnosis of the retinal alterations surrounding RAP lesions, it is limited in its ability to distinguish true inner retinal cysts from pseudocystic cavities. In the present study, whether inner retinal cysts found in RAP lesions were true cysts or pseudocystic, they were the second most commonly found lesion, after drusen (Table 2). Moreover, regardless of their size, CNV appeared to develop subsequently and adjacent to inner retinal cysts, as a manifestation of the progression to RAP.
Along with the neovascularization of new vessels growing from the intraretinal complex of RAP, scar tissue called fibrovascular proliferation as well as FVPED may form on the surface of the retina. The fibrovascular tissue may distort the overlying RPE and outer retinal barrier leading to the spread of new vessels into subretinal space or into the neurosensory retina, causing serous detachment of the retina [21,22]. On FA, FVPED appears stippled hyperfluorescence within irregularly elevated PED, which shows leakage of an undetermined source, also in a stippled pattern [11,22]. All of the cases with FVPED found in our study were complicated by SRD and/or PED.
ORCs are a new type of cystic structure recently identified in patients with AMD, and can be differentiated from intraretinal exudates and cystoid cavities lying in the outer plexiform layer by their surrounding hyperreflective rings [15]. Zweifel et al. [23] reported that tubulations in the outer retinal layer result from sublethal injury to the photoreceptors and disruption of the RPE layer. When outer retinal cystoid changes are observed in patients with RAP, vision- threatening conditions should be considered in differential diagnosis to determine the most appropriate course of treatment.
Serous detachments of the RPE appear as optically clear areas between the RPE and the choriocapillaris, and a detachment can be single or, multiple, dome-shaped, or bilobed [24]. When RAP reaches the subretinal space and merges with the RPE, a serous detachment of the RPE will develop [2,25]. SRD demonstrates leakage of fluorescein in the corresponding area on FA and subsequent subretinal concretions may be indicative of spontaneously resolved previous serous detachments [3,4]. The progression of RAP on OCT is characterized by the presence of intraretinal (well-defined confluent hyporeflective) spaces or subretinal fluid (a well-defined, hyporeflective space between the neurosensory foveal retina and other highly reflective bands corresponding to the RPE) [2].
PED appears to be a dome-shaped, optically empty space lined by a highly reflective layer of RPE. Serous PED can often be found in the macular area where CNV lies at the margin or within the PED, and on ICGA, it can be revealed as a variable, minimal blockage of normal choroidal vessels usually evident in the midphase [14]. Sato et al. [26] suggested that the low height of small PED may indicate that the detached RPE and Bruch's membrane are connected by CNV.
In a comparison of BCVA, patients with FVPED and PED showed relatively lower visual acuity than patients with inner retinal cyst, outer retinal cystoid change and SRD at initial visit. Moreover, those groups with lower initial BCVA did not show improved BCVA at final visit and still showed lower levels of visual acuity regardless of the conventional treatment of RAP (Table 2). However, analyzing the BCVA of patients in this study may not be meaningful, since the six OCT findings appeared in combinations of at least two findings, with drusen present in all cases. BCVA may not be a reliable parameter in predicting the prognosis of OCT findings. However, it may be used as a reference point to evaluate whether more aggressive treatment should be pursued based on the type of OCT finding. Thus, the course of treatment for RAP patients who have FVPED and PED as demonstrated by OCT should be carefully considered, as they tend to show lower BCVA than patients with other findings.
In conclusion, we analyzed OCT findings of RAP patients and revealed six different types of lesions distinct to RAP. These findings may be a useful tool in diagnosis, elucidating the clinical course of the disease, choosing an appropriate course of treatment and predicting prognosis. In such lesions, OCT provides more accurate information than FA or high speed ICGA, and it can be preferable to other diagnostic tools in understanding RAP. Moreover, both inner retinal cysts and FVPED commonly occur in patients with RAP, yet only inner retinal cysts as an early finding, may be a predictive of development to RAP, since FVPED is more likely to appear in more advanced stages. Limitations of this study include its retrospective nature, the relatively small sample size, short follow-up period and lack of anatomic landmarks in scanning and analyzing OCT. Further large, prospective studies based on SD-OCT technology with long follow-up periods may be necessary to discover more features of RAP that can support our findings of this study.
REFERENCES
1. Dell'Omo R, Cassetta M, dell'Omo E, et al. Aqueous humor levels of vascular endothelial growth factor before and after intravitreal bevacizumab in type 3 versus type 1 and 2 neovascularization: a prospective, case-control study. Am J Ophthalmol 2012;153:155-161.e2.


2. Brancato R, Introini U, Pierro L, et al. Optical coherence tomography (OCT) angiomatous prolifieration (RAP) in retinal. Eur J Ophthalmol 2002;12:467-472.

3. Rouvas AA, Papakostas TD, Ntouraki A, et al. Angiographic and OCT features of retinal angiomatous proliferation. Eye (Lond) 2010;24:1633-1642.


4. Yannuzzi LA, Negrao S, Iida T, et al. Retinal angiomatous proliferation in age-related macular degeneration. Retina 2001;21:416-434.


5. Hartnett ME, Weiter JJ, Garsd A, Jalkh AE. Classification of retinal pigment epithelial detachments associated with drusen. Graefes Arch Clin Exp Ophthalmol 1992;230:11-19.


6. Kuhn D, Meunier I, Soubrane G, Coscas G. Imaging of chorioretinal anastomoses in vascularized retinal pigment epithelium detachments. Arch Ophthalmol 1995;113:1392-1398.


7. Hartnett ME, Weiter JJ, Staurenghi G, Elsner AE. Deep retinal vascular anomalous complexes in advanced age-related macular degeneration. Ophthalmology 1996;103:2042-2053.


8. Slakter JS, Yannuzzi LA, Schneider U, et al. Retinal choroidal anastomoses and occult choroidal neovascularization in age-related macular degeneration. Ophthalmology 2000;107:742-753.


9. Lafaut BA, Aisenbrey S, Vanden Broecke C, Bartz-Schmidt KU. Clinicopathological correlation of deep retinal vascular anomalous complex in age related macular degeneration. Br J Ophthalmol 2000;84:1269-1274.



10. Yannuzzi LA, Slakter JS, Sorenson JA, et al. Digital indocyanine green videoangiography and choroidal neovascularization. Retina 1992;12:191-223.


11. Yannuzzi LA, Hope-Ross M, Slakter JS, et al. Analysis of vascularized pigment epithelial detachments using indocyanine green videoangiography. Retina 1994;14:99-113.


12. Wolf S, Wolf-Schnurrbusch U. Spectral-domain optical coherence tomography use in macular diseases: a review. Ophthalmologica 2010;224:333-340.


13. Susan BB, Neil M, Bressler . Age-related macular degeneration: non-neovascular early AMD, intermediate AMD, and geographic atrophy. In: Schachat AP, Ryan SJ, Retina. 5th ed. London: Elsevier; 2013. p. 1161.
14. Gass JD. Serous retinal pigment epithelial detachment with a notch: a sign of occult choroidal neovascularization. Retina 1984;4:205-220.


15. Wolff B, Maftouhi MQ, Mateo-Montoya A, et al. Outer retinal cysts in age-related macular degeneration. Acta Ophthalmol 2011;89:e496-e499.


16. Fernandes LH, Freund KB, Yannuzzi LA, et al. The nature of focal areas of hyperfluorescence or hot spots imaged with indocyanine green angiography. Retina 2002;22:557-568.


17. Zacks DN, Johnson MW. Retinal angiomatous proliferation: optical coherence tomographic confirmation of an intraretinal lesion. Arch Ophthalmol 2004;122:932-933.


18. Chan WM, Lai TY, Lai RY, et al. Half-dose verteporfin photodynamic therapy for acute central serous chorioretinopathy: one-year results of a randomized controlled trial. Ophthalmology 2008;115:1756-1765.


19. Khanifar AA, Koreishi AF, Izatt JA, Toth CA. Drusen ultrastructure imaging with spectral domain optical coherence tomography in age-related macular degeneration. Ophthalmology 2008;115:1883-1890.



20. Cohen SY, Dubois L, Tadayoni R, et al. Prevalence of reticular pseudodrusen in age-related macular degeneration with newly diagnosed choroidal neovascularisation. Br J Ophthalmol 2007;91:354-359.


21. Leveziel N, Puche N, Richard F, et al. Genotypic influences on severity of exudative age-related macular degeneration. Invest Ophthalmol Vis Sci 2010;51:2620-2625.


22. Liakopoulos S, Ongchin S, Bansal A, et al. Quantitative optical coherence tomography findings in various subtypes of neovascular age-related macular degeneration. Invest Ophthalmol Vis Sci 2008;49:5048-5054.



23. Zweifel SA, Engelbert M, Laud K, et al. Outer retinal tubulation: a novel optical coherence tomography finding. Arch Ophthalmol 2009;127:1596-1602.


24. Doukas J, Mahesh S, Umeda N, et al. Topical administration of a multi-targeted kinase inhibitor suppresses choroidal neovascularization and retinal edema. J Cell Physiol 2008;216:29-37.



Fig. 1
A 66-year-old man with retinal angiomatous proliferation. (A) Fundus photograph showing drusen, which appears as: confluent yellowish spots on the macula (red arrow). (B) Fluorescein angiogram revealing hyperfluent, ill-defined confluent lesions including focal hyperpigmentation of the macula (arrow). (C) Indocyanine green angiogram showing small drusen, which are mildly hyperfluorescent or not clearly seen (black arrow). (D) Optical coherence tomography scan showing incontiguous elevation of the retinal pigment epithelium (RPE) with slight thickening of RPE/Bruch's membrane complex (dotted arrow).
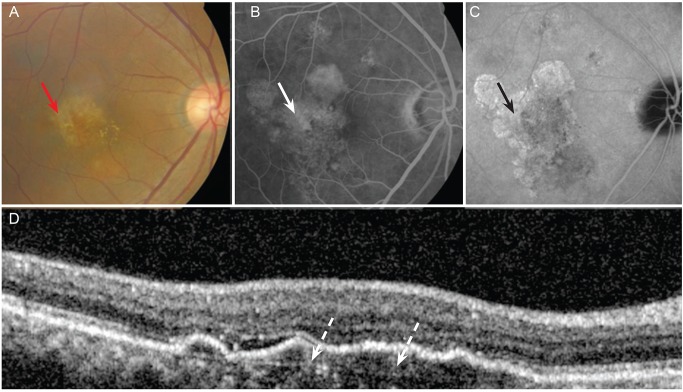
Fig. 2
A 54-year-old man with retinal angiomatous proliferation. (A) Fundus photograph revealing a delicate, star-shaped distortion of the macula without prominent cyst formation (red arrow). (B,C) Fluorescein and indocyanine green angiogram demonstrating retinal distortion, though leakage of dye is not found (arrows). (D) Optical coherence tomography scan showing round, minimally reflective (darker) space spanning nearly the entire thickness of the retina and extending from the retinal pigment epithelium/choriocapillaris reflection to the highly reflective anterior boundary of the neurosensory retina (dotted arrow).
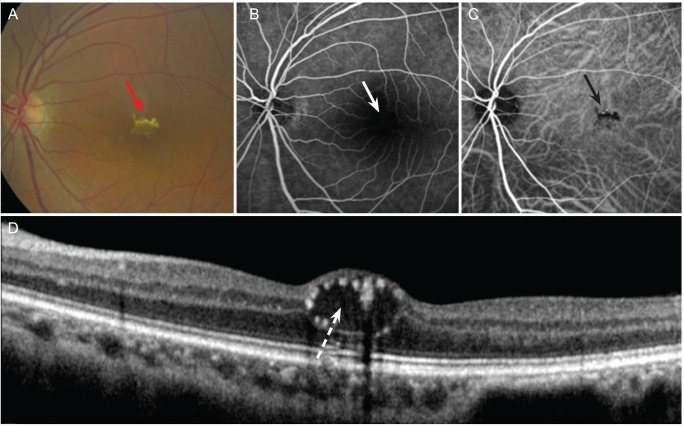
Fig. 3
A 61-year-old woman with retinal angiomatous proliferation. (A) Fundus photograph showing distortion of the macula with yellowish scar change surrounding a cyst-like lesion (red arrow). (B) Fluorescein angiogram revealing dense hyperfluorescence with diffuse leakage of dye in cystic spaces near, but not inside, the fovea (arrow). (C) Indocyanine green angiogram showing the presence of a RAP, which is classified as an irregular hyperfluorescence with termination of the retinal vasculature (arrow head). (D) Optical coherence tomography scan showing subretinal tissue presumably corresponding to the yellowish scar change visible on the color photo (dotted black arrow). Note the inner retinal cystoid cavities above.
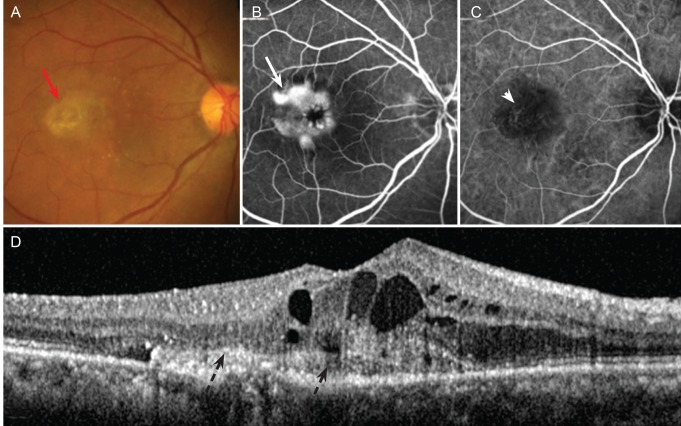
Fig. 4
A 65-year-old woman with retinal angiomatous proliferation. (A) Fundus photograph showing diffuse, patch-like cystic change underneath the retinal pigment epithelium in the macula (red arrow). (B) Fluorescein angiogram showing small hyperfluorescence with diffuse leakage of dye in the cystic spaces near and inside the fovea with stippled hyperfluorescence beneath the fovea (arrow). (C) Indocyanine green angiogram revealing the presence of a retinal angiomatous proliferation, which is classified as an irregular hyperfluorescence (black arrow). (D) Optical coherence tomography scan showing two adjacent outer retinal cysts (ORCs) located in a fibrotic area associated with choroidal neovascularization, which is surrounded by a hyperreflective border (dotted arrow). Note the differences between the ORCs and the inner retinal cystoid cavities above.
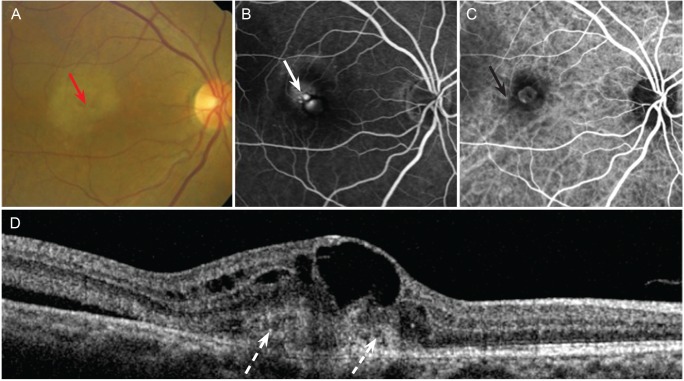
Fig. 5
A 55-year-old woman with retinal angiomatous proliferation. (A) Fundus photograph showing distortion of the macula with yellowish patch-like lesions surrounded by broad cystic change (red arrow). (B) Fluorescein angiogram revealing dense hyperfluorescence with diffuse leakage of dye mimicking choroidal neovascularization in the macula. A large cystic lesion lies inferotemporally, but cannot be clearly seen (arrow). (C) Indocyanine green angiogram showing a more prominent boundary of cystic space below the macula (black arrow). (D) Optical coherence tomography scan indicating subretinal fluid (dotted arrow) adjacent to the subretinal tissue.

Fig. 6
A 64-year-old woman with retinal angiomatous proliferation. (A) Fundus photograph showing a serous retinal pigment epithelium detachment and subretinal hemorrhage (red arrow). (B,C) Fluorescein and indocyanine green angiogram showing dye leakage from choroidal neovascularization within the retinal pigment epithelial detachment (arrow and arrowhead). (D) Optical coherence tomography scan revealing the dome-shaped elevation of a highly reflective layer corresponding to the detached retinal pigment epithelium (dotted arrow).





 PDF Links
PDF Links PubReader
PubReader Full text via DOI
Full text via DOI Full text via PMC
Full text via PMC Download Citation
Download Citation Print
Print




