 |
 |
| Korean J Ophthalmol > Volume 26(4); 2012 > Article |
Abstract
Lacrimal sac diverticulum is a rare condition, and its various symptoms complicate differential diagnosis. We present cases of a peculiar type of lacrimal diverticulum. A 5-year-old girl and a 50-year-old woman presented with a protruding mass inferior to the medial canthus. Each lacrimal system was patent to irrigation. The masses compressed and distorted the lacrimal passage and had no apparent connection with the lacrimal sac in dacryocystography or computed tomography. Surgical exploration and complete excision of the masses were completed. Each patient had an inverted Y- and an inverted V-shaped multilobular cystic mass that was pathologically confirmed as a lacrimal sac diverticulum. Lacrimal sac diverticula may rarely take the form of a multilobular cyst and can present as a lower lid mass. We speculate that an abnormality in lacrimal embryogenesis resulted in multiple blind pouches, a peculiar type of lacrimal sac diverticulum.
Lacrimal sac diverticulum is a protruded pouch that generally exhibits communication with the lacrimal sac [1]. The pathology may cause epiphora, discharge, pain, and result in a fluctuating mass and cutaneous erythema. Usually, such a diverticulum is asymptomatic and is occasionally diagnosed with dacryocystography [2]. The lacrimal sac diverticulum may be of congenital, inflammatory, or traumatic origin [3]. Congenital origin should be suspected if there is no history of trauma or inflammation of the lacrimal sac.
In this study, we present two cases of a distinctive type of lacrimal diverticulum consisting of 2 to 3 lobules with patent lacrimal drainage system and presenting as a lower eyelid mass. This is a new description of the morphologic characteristics of a lacrimal diverticulum.
A 5-year-old girl visited our clinic with a mass on the right lower eyelid for 10 days. She did not have a history of lacrimal obstruction, dacryocystitis, or trauma. She had mild epiphora and conjunctival discharge of the right eye. The non-tender, ovoid mass was fixed along the medial portion of the inferior orbital rim (Fig. 1A). It was not reducible and felt like an air-fluid mixture upon palpation. The lacrimal outflow system showed no obstruction upon lacrimal irrigation. Dacryocystography (Fig. 1B and 1C) and an orbital computed tomography (CT) scan were performed (Fig. 1D and 1E).
Under general anesthesia, exploration was performed using a subciliary eyelid incision. The mass was completely excised. From the operative findings, an inverted Y-shaped cystic mass was identified on the lateral side of the lacrimal sac. The lateral lobule, 1.2 cm long in the long axis, extended along and was firmly attached to the inferior orbital rim. The inferior rim of the bony orbit was remodeled and had a bony depression along the lobule. The inferior lobule infiltrated 3 mm into the nasolacrimal bony canal and medially displaced the nasolacrimal duct. The superior lobule stretched upward and around the lacrimal sac posteriorly and medially. The lobule also pushed the lacrimal sac anteriorly and laterally (Fig. 1B). The mass was adherent to the lateral wall of the lacrimal sac at the center of the three lobules. There was fibrotic tissue between the mass and the lacrimal sac without visible communication. In the histological examination, the wall of the mass consisted of pseudostratified cuboidal and pseudostratified columnar epithelia (Fig. 1F). These findings were compatible with a lacrimal diverticulum or cyst originating from the lacrimal sac.
The patient did not exhibit any tearing symptoms or mass recurrence after 12 months of follow-up.
A 50-year-old woman presented with a lower eyelid mass and epiphora for 2 months. She did not have any tearing symptoms or a history of dacryocystitis. The mass was firm and fixed to the inferior orbital rim. The overlying skin showed erythematous change (Fig. 2A). There was no tenderness, and no regurgitation could be elicited upon digital compression. The lacrimal drainage system was patent during lacrimal irrigation. Dacryocystography (Fig. 2B and 2C) and CT of the orbit were performed (Fig. 2D and 2E).
The mass was completely excised and consisted of inverted V-shaped lobules in the operative findings. The lateral lobule extended along the inferior orbital rim, to which its inferior border was fixed. The inferior lobule penetrated 3 mm into the nasolacrimal bony canal. The apex of the mass was firmly attached to the lateral wall of the lacrimal sac. A dacryolith was found in the cavity of the inferior lobule, which was compatible with a high density in the CT (Fig. 2E). The patient did not present epiphora or mass recurrence after 6 months of follow-up.
The two cases showed a distinct type of cystic mass attached to the lacrimal sac. The masses consisted of two to three lobules extending along the inferior orbital rim and the nasolacrimal canal in both cases and extending to the lacrimal sac fossa in one case. Despite a report of a diverticulum that grew into the inferior orbital rim, most diverticulae arise in the lateral wall of the lacrimal sac as a single pouch [4,5]. The inferior part of the lateral wall is the most vulnerable site for diverticulum since the medial wall is surrounded by the periosteum, and the superior portion of the lacrimal sac is enforced by the orbicularis muscles and the medial canthal tendon. In our two cases, the inferior portion of the lateral wall was the origin of the diverticulum.
Diverticulum growing along the bony wall around the lacrimal sac is an interesting feature. The reason for its presence along the bony wall is not clear. We can speculate that some growth factors from the periosteum may have an inductive effect on cyst elongation and adhesion.
There was no apparent connection between the lacrimal sac and either of the masses in dacryocystography. However, there was some evidence of clinical communication: there was inflammation due to an ascending infection in both cases. In the first case, the pouch contained an air-fluid mixture and the mass fluctuated in size. It could be speculated that there may be a valve-like structure between the mass and the lacrimal sac [3].
Embryologically, the lacrimal outflow system arises from the cellular cord of ectoderm between the maxillary and frontonasal processes in the 6-week-old embryo. Canalization in the buried ectoderm cord gives rise to the lacrimal outflow system [6]. An abnormal cellular cord stem could be established during embryogenesis, and a lacrimal sac fistula and an outpouching from the lacrimal sac can be formed [7]. If communication between the congenital lacrimal sac diverticulum and the lumen of the lacrimal sac is hindered, this outpocket becomes a cyst of the orbit [8].
When a lower eyelid mass exhibits evidence of a connection with the lacrimal sac or is fluctuating in size, a lacrimal sac diverticulum should be considered. Lacrimal sac diverticulae of congenital origin can take on a multilobular form and may have various radiological imaging features. Proper treatment should be tailored for each patient.
REFERENCES
1. Duke-Elder S, MacFaul PA. In: Duke-Elder S, The ocular adnexa: lacrimal, orbital, and para-orbital diseases. Cysts and diverticula. System of ophthalmology. Vol. 13. The ocular adnexa. 1974. St. Louis: CV Mosby; p. 733-735.
2. Polito E, Leccisotti A, Menicacci F, et al. Imaging techniques in the diagnosis of lacrimal sac diverticulum. Ophthalmologica 1995;209:228-232.


5. Akcay EK, Cagil N, Yulek F, et al. Congenital lacrimal sac diverticulum as a cause of recurrent orbital cellulitis. Can J Ophthalmol 2009;44:e29-e30.


6. Hurwitz JJ. In: Hurwitz JJ, Embryology of the lacrimal drainage system. The lacrimal system. 1996. Philadelphia: Lippincott-Raven; p. 9-13.
Fig.┬Ā1
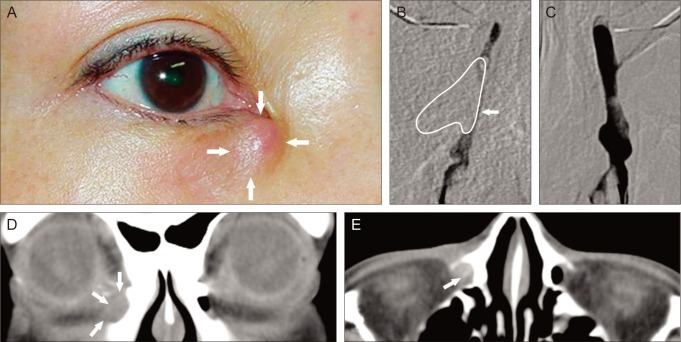
Case 1. (A) A mass was found along the right inferior orbital rim (arrows). (B) Dacryocystography was performed. A reconstructed image of an inverted Y-shaped mass (white line): the lateral lobule extended along the inferior orbital rim, the inferior lobule pushed the nasolacrimal duct medially (arrow), and the superior lobule displaced the lacrimal sac both anteriorly and laterally. There was no dye outflow across the lacrimal sac wall. (C) Dacryocystography of the left side. (D) Coronal computed tomography (CT): a soft tissue mass surrounded by rim enhancement (arrows). (E) Axial CT: air density (arrowhead) of the lacrimal sac was displaced anteromedially by the mass (arrows). The lacrimal sac fossa was widened. (F) Epithelium of the mass consisted of pseudo-stratified cuboidal and columnar epithelium. The wall of the mass consisted of fibroblasts and collagen fibers (H&E, ├Ś100).

Fig.┬Ā2
Case 2. (A) A lower eyelid mass fixed along the inferior orbital rim (arrows) with overlying skin erythema. (B) Dacryocystograph of the right side: a reconstructed image of an inverted V-shaped mass (white line) next to the right lacrimal sac and nasolacrimal duct. The mass was compressing the lacrimal sac and nasolacrimal duct (arrow). (C) Dacryocystograph of the left side. (D) Coronal computed tomography (CT): a soft tissue mass (arrows) compressed the lacrimal sac at the level of the medial canthus. (E) Axial CT: a high density inside the mass (arrow) at the level of the upper part of the nasolacrimal duct indicated dacryolithiasis at the inferior lobule of the diverticulum.
- TOOLS
-
METRICS

- Related articles
-
Orbital Sarcoidosis Presenting as Diffuse Swelling of the Lower Eyelid2013 February;27(1)



 PDF Links
PDF Links PubReader
PubReader Full text via DOI
Full text via DOI Full text via PMC
Full text via PMC Download Citation
Download Citation Print
Print



