 |
 |
| Korean J Ophthalmol > Volume 26(2); 2012 > Article |
Abstract
This retrospective observational case series on eyes from three patients was done to elucidate the developmental mechanism of spontaneous reattachment of rhegmatogenous retinal detachment (SRRRD). The study eyes of each patients showed evidence of retinal break and diffuse retinal pigmentary change. Ultrasound biomicroscopic examination revealed vitreous fibers attached to the area around the retinal break. Posterior vitreous attachment was confirmed in each eye. A thin fibrovascular membrane incompletely sealing the retinal break was noted in one case. We suggest that the vitreous attachment around the retinal break and the sealing of the break with adjacent vitreous fibers seem to be involved in the developmental mechanism of SRRRD.
Rhegmatogenous retinal detachment is a progressive condition and usually requires surgical intervention. Spontaneous reattachment of rhegmatogenous retinal detachment (SRRRD) is a rare phenomenon, initially described by Cantrill in 1981 [1], with only a few SRRRD case series being reported since then [2-4]. We recently described the clinical characteristics of SRRRD [4], however, the developmental mechanism of SRRRD has not been clarified. After our prior published case series, we observed an additional 10 cases of SRRRD. Among them, three cases exhibited retinal breaks within the SRRRD lesion. In those cases, the factors related to the developmental mechanism of SRRRD have been sought. Herein, we report on cases that may suggest a developmental mechanism of SRRRD.
An asymptomatic 22-year-old female was referred to our clinic with a diagnosis of fundus abnormality left eye (OS) detected upon preoperative examination prior to refractive surgery. Visual acuity was 20 / 20 both eyes (OU). Refractive error was -7.5 Dsph right eye (OD) and -5.75 Dsph OS. Dilated fundus examination OS revealed an old, localized retinal detachment with a demarcation line and lattice degeneration, with a retinal hole in the inferior temporal periphery. Pigmentary changes were conspicuous, with a convex margin at the attached retina posterior to the demarcation line (Fig. 1A). SRRRD was diagnosed. Ultrasound biomicroscopic (UBM 840; Zeiss-Humphrey, Jena, Germany) examination of the retinal periphery near the causative retinal hole revealed vitreous fibers both anterior and posterior to the retinal hole (Fig. 1B and 1C). No change in retinal lesions was observed over a follow-up period of two years.
A 58-year-old male was referred to our clinic with a diagnosis of fundus abnormality OD. The patient complained of blurred vision lasting several months. Visual acuity was 20 / 30 OD and 20 / 20 OS. Refractive error was -1.75 Dsph OD and -2.0 Dsph OS. Dilated fundus examination OD revealed a pigmented peripheral retinal lesion with convex margin at the 6-o'clock position of the peripheral retina. One disc-sized retinal hole was detected within the lesion (Fig. 2A). The patient was diagnosed with SRRRD and a suspected macular epiretinal membrane. Optical coherence tomographic (OCT; Cirrus, Carl Zeiss Meditec, Dublin, CA, USA) examination revealed that the presumed epiretinal membrane was actually a thickened posterior hyaloid membrane. It was also determined that partial posterior vitreous detachment (PVD) had developed only on the temporal side of the fovea (Fig. 2B and 2C). The patient underwent a pars plana vitrectomy to relieve macular edema due to vitreous traction. Posterior vitreous attachment was confirmed intraoperatively.
An asymptomatic 38-year-old male was referred to our clinic with a diagnosis of retinal break OD, which was incidentally detected when the patient underwent a scleral buckling operation in the fellow eye. Visual acuity was 20 / 25 OU. Dilated fundus examination OD revealed a pigment-stippled peripheral retinal lesion with a convex margin from 7-o'clock to 11-o'clock. The appearance of the right eye was consistent with a diagnosis of SRRRD. A two disc-diameter sized horseshoe tear with a rolled edge was noted at the 8-o'clock position of the peripheral retina, within the SRRRD lesion. The retinal tear was covered and incompletely sealed by a thin translucent vascularized membrane (Fig. 3A). UBM examination showed vitreous fibers and a membranous structure overlying the retinal tear (Fig. 3B and 3C). Evidence of PVD, including a Weiss ring, was not observed.
Findings for all three patients were consistent with SRRRD, including retinal pigmentary alterations with convex margin of the retinal lesion. Interestingly, UBM examination in case 1 revealed vitreous fibers attached to the retinal hole at both the posterior and anterior margins. OCT in case 2 demonstrated that a PVD developed only at the horizontal meridian, suggesting vitreous attachment at the optic disc and elsewhere. In addition, posterior vitreous attachment was confirmed intraoperatively in case 2. Thus, it seems most likely that PVD was not present in the inferior retinal periphery, where the SRRRD was observed. Retinal detachments may develop in the absence of a PVD, as was noted in the retinal detachment due to atrophic holes within lattice degeneration [5]. This finding has been shown to occur in younger patients with myopia [5]. However, the development of retinal detachment in the absence of a PVD is apparently a rare event.
Based on our observations, we suspect that the developmental mechanisms of SRRRD are as follows. Initially, both focal vitreoretinal adhesion and vitreoretinal traction induce a retinal break in the peripheral retina in an eye without a complete PVD (as in cases 2 and 3). This is followed by an influx of liquefied vitreous into the retinal break, constituting the development of retinal detachment. However, the direction of vitreoretinal traction changes to parallel the elevated retinal surface (as in case 1). Eventually, vitreoretinal traction is relieved and the retinal break is closed by vitreous fibers running parallel to the retinal plane. This is especially likely if there is vitreous attachment at the posterior border of the retinal break, as in case 1. As with the interruption of fluid currents through the subretinal space, SRRRD develops, and the thin membrane proliferates over the retinal break (case 3). Proliferative membrane sealing of the retinal break as a form of wound healing response contributes to the induction and/or maintenance of retinal reattachment. We suspect the proliferative membrane results from fibroglial and retinal pigment epithelial hyperplasia.
In our current report of three cases with SRRRD, retinal breaks causing retinal detachment were identified. It is worthy to note that the localization of the retinal break in the eyes that developed SRRRD is apparently a rare event. Despite an extensive search, a retinal break was not identified in any of the 15 cases in a previous series [4]. Results of our current study lend indirect support to the prior contention that SRRRD preferentially develops in cases of retinal detachment with a small retinal break. Identification of a small causative retinal hole would be difficult once development of SRRRD is complete, due to the bridging of thin fibrous tissue over the small retinal hole. In addition, diffuse retinal pigment atrophy and sub- and/or an epiretinal membrane within the extent of SRRRD could hinder detection of a small retinal hole.
In conclusion, we determined that the incidence of SRRRD appears closely related to the absence of a PVD near the retinal break, as well as to membrane proliferation over the retinal break.
Fig. 1
Left eye in patient 1. (A) Fundus photograph at presentation: pigmentary clumping and atrophy at the attached retina (solid white arrow heads) posterior to the area of retinal detachment (empty arrow heads) with a retinal hole (black arrow). (B,C) Ultrasound biomicroscopic examination disclosed vitreous fibers (white arrows) both anterior and posterior to the retinal hole.
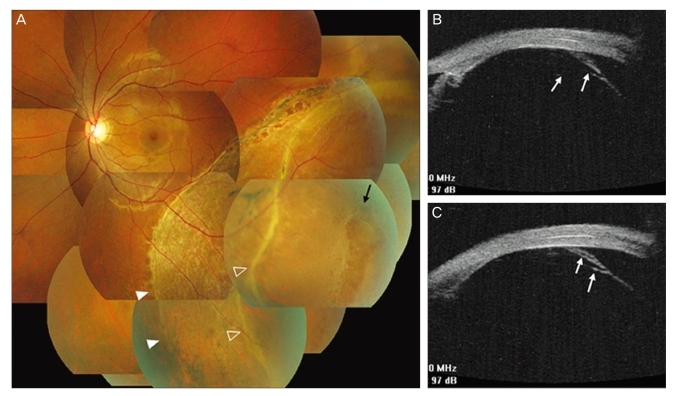
Fig. 2
Right eye in patient 2. (A) Notice the retinal pigmentary alteration and retinal hole (black arrow) at the 5-o'clock position. (B,C) Optical coherence tomographic examination revealed development of posterior vitreous detachment on the temporal side of the fovea only.
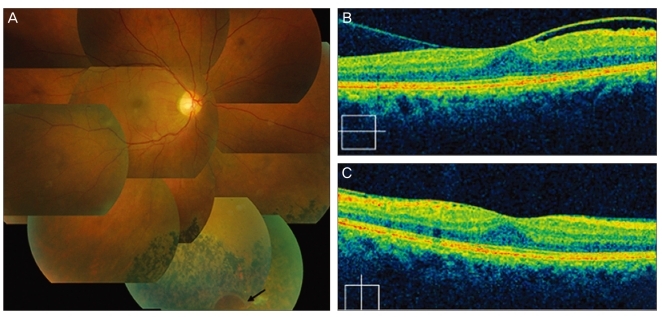
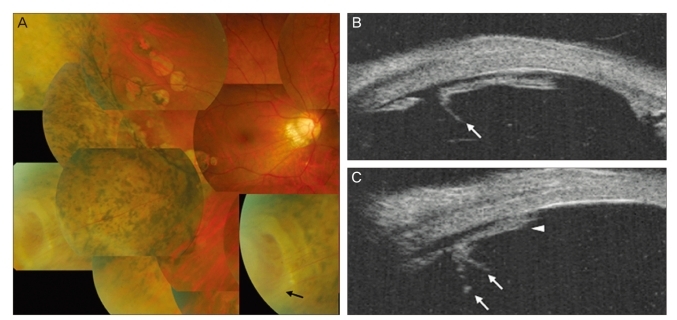
Fig. 3
Right eye in patient 3. (A) Fundus photograph at presentation shows extensive retinal pigmentary clumping, atrophy, and a 2 disc-diameter horseshoe retinal tear at the 8-o'clock position. The magnified image reveals thin fibrovascular membrane (black arrow) connecting the anterior and posterior margins of the retinal tear. (B,C) Ultrasound biomicroscopic imaging showed vitreous fibers (white arrows) and membranous structure sealing the retinal tear (white arrow head).
- TOOLS
-
METRICS

- Related articles
-
Reattachment of Rhegmatogenous Retinal Detachment via Fibrin Tissue Adhesive2021 June;35(3)
Impact of Age on Scleral Buckling Surgery for Rhegmatogenous Retinal Detachment2017 August;31(4)
Macular Hole Formation in Rhegmatogenous Retinal Detachment after Scleral Buckling2014 October;28(5)



 PDF Links
PDF Links PubReader
PubReader Full text via DOI
Full text via DOI Full text via PMC
Full text via PMC Download Citation
Download Citation Print
Print



