 |
 |
| Korean J Ophthalmol > Volume 25(5); 2011 > Article |
Abstract
Purpose
To assess long-term anatomic and visual outcomes and associated complications of lens-sparing vitrectomy (LSV) for treatment of tractional retinal detachments (TRDs) associated with stages 4B and 5 retinopathy of prematurity (ROP).
Methods
We performed a retrospective review of medical records and data analyses of consecutive patients who presented with stages 4B and 5 ROP and underwent LSV from 1999 to 2007. Retinal reattachment status, visual acuity and postoperative complications were evaluated.
Results
Twenty-one eyes of 20 patients, including 13 eyes with stage 4B ROP and 8 eyes with stage 5 ROP, were examined. The mean follow-up period was 5.6 years. In 9 (43%) out of 21 eyes, retinas were eventually reattached. The anatomic success rates were 62% in stage 4B and 13% in stage 5 ROP. In eyes with reattached retinas, visual acuity better than form vision was shown in 7 eyes (78%), whereas no light perception was present in 10 eyes (83%) among eyes with TRD on final examination. Postoperative intraocular hemorrhage occurred in nine eyes (43%). Long-term complications of cataract, corneal opacity, glaucoma and strabismus developed in 4 (19%), 6 (29%), 7 (33%) and 8 (38%) eyes, respectively, and were more common in eyes with TRD.
Conclusions
After following-up for a mean of 5.6 years, the anatomical success rate of LSV was encouraging for the correction of TRD associated with stage 4B ROP but not for stage 5 ROP. Retinal reattachment is important for obtaining better visual outcomes and preventing the development of late complications.
Retinal detachments associated with retinopathy of prematurity (ROP) have poor anatomical and visual prognoses [1,2], and treatment for stages 4 and 5 ROP includes scleral buckling (SB) [3-6] and vitrectomy with or without lensectomy [7-9]. Although the stage, extent and location of tractional retinal detachments (TRDs) and the presence or absence of retina-lens apposition are considered when making a surgical decision, controversies concerning when the surgery should be performed and which surgical techniques are the most beneficial for the treatment of TRDs in stage 4 and 5 ROP still exist. Since Capone and Trese [10] suggested that lens-sparing vitrectomy (LSV) for stage 4A ROP reduced disease progression and improved the patients' visual prognosis, LSV has been widely used in stages 4 and 5 ROP and has yielded favorable anatomical and visual outcomes, especially in stage 4 ROP [11-23]. In contrast, some authors have suggested that LSV fails to prevent the progression of retinal detachment in cases of aggressive posterior ROP because of insufficient removal of the vitreous gel at the vitreous base, as compared to lensectomy and vitrectomy (LV) in which the gel is completely removed [24].
The anatomical success of LSV was found to be favorable in previous studies. However, follow-up periods ranged from six months to three years [10-23]. Even after successful retinal reattachment by LSV, retinal detachment can occur after variable time intervals and vitrectomy for immature eyes can cause complications such as corneal opacity, cataracts and growth retardation of the eyeball [25]. The long-term anatomical and visual outcomes and the prevalence of the complications of LSV remain unknown and require further study.
In 2006, Yu et al. [19] reported the anatomical and visual results of LSV for Korean infants with stages 4 and 5 ROP after a mean postoperative follow-up period of 2.2 years. They suggested that LSV had encouraging surgical outcomes for the correction of retinal detachment associated with ROP, especially in stage 4 ROP eyes. Four years later, we felt the need to investigate and report the long-term outcomes of LSV, including its long-term complications, in stages 4 and 5 ROP after continuous patient follow-up. The purpose of the current study was to report the long-term outcomes of LSV for the treatment of retinal detachment associated with ROP in consecutive cases in Korea.
Patients who underwent LSV for posterior-type stages 4B and 5 ROP in at least one eye at Seoul National University Children's Hospital between 1999 and 2007 and who underwent follow-up for more than 24 months postoperatively were enrolled in this study, including patients who had previously been enrolled in the study reported by Yu et al. [19]. We reviewed the medical records of these patients retrospectively. Preoperative clinical findings, including patients' gestational age at birth, birth weight, gender, treatment history before LSV, ROP status (including stage and presence or absence of plus disease at the time of LSV), postoperative results (including anatomic result, visual acuity and any complication encountered after LSV), and further treatment history, were examined. The stages of ROP were defined in accordance with the international classification of ROP and plus disease (vascular dilation and tortuosity in at least two quadrants of the posterior pole) [26]. Written informed consent was obtained from the parents of all participants before examinations under anesthesia and LSV were conducted.
The decisions of surgery and types of surgical procedures were made by an experienced pediatric retinal surgeon (YSY), and the surgical techniques for LSV were the same as those described by Maguire and Trese [27]. Surgery was completed after removing as much of the tractional membrane as possible and letting the entire retina be free from traction without any injury to the lens. Intra-vitreal air injection was performed at the end of the surgery to maintain eyeball pressure.
Postoperatively, all patients were examined in the clinic by the surgeon (YSY). Visual rehabilitation was performed as necessary. Follow-up examinations were conducted periodically to monitor the retinal status and vision and to identify cataracts, cornea opacity, glaucoma, microphthalmia, and strabismus. Anatomical success was defined as at least an attachment of the retina at the posterior pole at the last follow-up [19]. Final vision was classified into categories: favorable vision including a visual acuity of 20 / 2000 or better and form vision (patients can fix their eyes on a small moving toy and follow the moving toy); unfavorable vision including light follow (patients can fix their eyes on a moving pen-light), light perception (patients can differentiate between the light-on and -off), and no light perception [19].
Statistical analyses were performed using the SPSS ver. 17.0 (SPSS Inc., Chicago, IL, USA).
Twenty-one eyes of 20 patients were enrolled in this study. They consisted of 10 males and 10 females and 11 right eyes and 10 left eyes. The mean gestational age at birth of patients was 29+0 weeks (range, 25+0 to 33+4 weeks), and the mean birth weight of patients was 1,284 g (range, 640 to 2,340 g). All eyes were treated with peripheral ablation with laser photocoagulation and/or cryotherapy, and two eyes underwent additional scleral buckling and encircling before LSV. The mean gestational age at surgery was 44+1 weeks (range, 35+4 to 64+2 weeks). Patients were followed-up for a mean of 5.6 years (range, 2.5 to 9.3 years), and the mean age of patients at the last follow-up was 5.8 years (range, 2.7 to 9.5 years) (Table 1).
Table 2 lists the demographics and outcomes of LSV in individual patients. Thirteen eyes of 12 patients were found have stage 4B ROP, and 8 eyes of 8 patients had stage 5 ROP at the time of LSV. Plus diseases were observed in 12 eyes (92%) with stage 4B ROP and 2 eyes (25%) with stage 5 ROP. The mean gestational age at birth and birth weight were similar between the two groups (p = 0.440 and 0.143, respectively, by Mann-Whitney U-test). The age at the time of LSV also was insignificant between the groups (p = 0.015). Anatomical reattachment of the retina was achieved after a single LSV procedure in seven eyes (54%) with stage 4B ROP and one eye (13%) with stage 5 ROP. Of the stage 4B ROP eyes, two eyes underwent an additional LV, and the retina was successfully reattached in one eye. Among the stage 5 ROP eyes, two underwent an additional LV procedure, but the retina was not successfully reattached in either patient. Therefore, the overall anatomical success rate of LSV in our clinic was reported as 43%, which included eight eyes (62%) with stage 4B ROP and one eye (13%) with stage 5 ROP (Table 3). The presence or absence of plus disease was not found to affect anatomical success or failure of the LSV procedure (p = 0.134). Lensectomy was used to treat four eyes with persistent TRD due to secondary pupillary-block glaucoma.
Immediately after surgery, a retinal tear was found in only one eye (5%), and intraocular hemorrhage, including vitreous hemorrhage and/or preretinal hemorrhage, was found in nine eyes (43%); all hemorrhages later resolved. No lens injury or cataracts were detected. However, complications developed over a period of time. Cataracts were found in four eyes (19%); corneal opacity in six eyes (29%); secondary pupillary-block glaucoma in seven eyes (33%); microphthalmia in one eye (5%); and strabismus in eight eyes (38%) (Table 4).
The age at birth and birth weight were similar between the anatomical success and failure groups (p = 0.132, 0.537). Also, the age at LSV of patients in the success group was similar to that of patients in the failure group (p = 0.749). The final visual outcome was found to be better for eyes in which the retinal attachment was successful than for the eyes in which the retina remained detached (p = 0.002, by Fisher's exact test). Of the eyes with reattached retinas, all had light perception, and 78% of the eyes exhibited favorable visual outcomes including form vision or a visual acuity of 20 / 2000 or better. However, of the eyes with detached retinas, 91% were found to have unfavorable visual outcomes either with or without the loss of light perception vision. Among the long-term complications associated with LSV, corneal opacity and secondary glaucoma developed only in the eyes with detached retinas (p = 0.017 and 0.007, respectively) (Table 5).
In their previous study, Yu et al. [19] reported an average anatomical success rate of 58.8% for LSV in 17 eyes with stages 4 and 5 ROP after a mean follow-up period of 2.2 years. The success rates of stages 4A, 4B and 5 ROP eyes were 75%, 66.7% and 25%, respectively. Form vision (when patients can fix their eyes on and follow a small moving toy) was found in six eyes (35%), light following was observed in three eyes (18%) and no light perception was found in eight eyes (47%) during the last follow-up examination [19]. Approximately four years after that study, we reviewed 21 eyes with stages 4B and 5 ROP. Eyes with stage 4A ROP were excluded from this study because the conditions were usually rapidly progressing posterior-type ROP with poor outcomes. Therefore, we analyzed the 4A ROP cases separately. All eyes were followed-up for more than 24 months with an average follow-up period of 5.6 years. Our study showed similar anatomical success rates and visual outcomes as a previous study for stages 4B and 5 ROP by Yu et al. [19]. The overall success rate of LSV in our study was 43%, and the success rate for stages 4B and 5 ROP was found to be 62% and 13%, respectively.
El Rayes et al. [22] reported an anatomical success rate of 75% in LSV for stage 4B ROP after a three-year follow-up period, which was lower than the LSV success rates reported for the same stage in other studies with a shorter follow-up period [14,16]. Kondo et al. [25] observed that after successful retinal reattachment by vitrectomy in patients between 2 and 10 years of age, retinal detachment recurred in 5% and 22% of stages 4B and 5 ROP eyes, respectively, especially when clear signs of traction, localized residual retinal detachment, peripheral retinal breaks, or dense vitreous hemorrhages were present. Therefore, patients with a longer follow-up who underwent LSV for TRD associated with ROP may have a lower anatomical success rate. We could not find any studies that compared the anatomical success rates of LSV according to the follow-up period in the same consecutive case series. Further, in our study, we did not identify any cases of late TRD recurrence after successful retinal reattachment. Because we relieved as much traction as possible during the surgical procedure, the residual traction was less.
Hartnett [28] suggested that the presence of plus disease at the time of LSV could be the cause of surgical failure. Although the presence or absence of plus disease did not affect the surgical outcomes in our study, it is possible that it had adverse effects on the surgical outcomes because it led to intraoperative and/or postoperative hemorrhage or new fibrovascular traction membranes. However, it is also plausible that if surgery is delayed until the plus disease regresses completely, the detachment could progress to total TRD or the retina could become too rigid to be reattached. In our study, although the incidence of plus diseases in the eyes with stage 5 ROP was low, a poorer anatomical success rate was observed as compared to that in other studies. Therefore, determining the appropriate time at which LSV should be performed is important for surgical success, although still controversial.
Once the retina detaches in eyes with ROP, visual outcomes are devastating even if anatomical reattachment is achieved. Studies have reported highly variable visual outcomes after LSV in eyes with ROP [11,13,18,19,22,23]. Lakhanpal et al. [18] found that that the mean visual acuity for stage 4B ROP after LSV was 20/200. El Rayes et al. [22] reported that after LSV or LV for stage 4B ROP, 97.4% of eyes achieved ambulatory vision (visual acuity better than 20 / 1900), and 42.8% of eyes achieved near reading vision (visual acuity better than 20 / 800). They also observed that retinal reattachment, LSV and pretreatment with retinal ablation were associated with better visual acuity [22]. In our study, a visual acuity of 20 / 2000 or better was achieved in only two eyes (9.5%), and form vision was noted in only six eyes (28.6%). The lower anatomical success rates and higher prevalence of late complications, such as corneal opacity (29%), cataracts (19%) and glaucoma (33%), that interrupted visual development might be the main causes of the poor overall visual outcomes. We are unaware of other reasons why we obtained poor visual outcomes despite achieving retinal reattachment.
Moshfeghi et al. [15] reported a low prevalence of complications with LSV, but the prevalence of complications was much higher in our study. To date, other than our study, no report has mentioned the complications associated with LSV in detail, especially the long-term complications, excluding cataracts. Because LSV requires a skilled surgical procedure and a long operative time, these factors could cause complications in the eyes of infants. Our report showed that retinal reattachment is very important not only for improving vision but also for preventing long-term complications such as corneal opacity, secondary glaucoma and microphthalmia, which occurred only in eyes with detached retinas.
Previous reports showed that SB for stage 4 ROP has reattachment rates of 46% to 75% [4-6,29-31], while LV for stage 4 ROP has reattachment rates of 64% to 84% [7-9,32]. Although our study showed poorer anatomical success rates as compared to other studies, the 43% reattachment rate we reported after a mean follow-up period of 5.6 years seems to be comparable to the outcomes reported for SB and LV. LSV has certain advantages over SB; it does not cause a myopic shift and does not require additional surgery for buckle removal, and the post-LSV phakic condition that aids visual rehabilitation is comparable to that after LV. Therefore, LSV can be an effective treatment option for TRD associated with ROP.
Nonetheless, our study has several limitations. It was a retrospective and non-comparative consecutive case series study that included a widely heterogeneous group of patients. The retinal conditions of the patients in this study differed widely at the time of surgery, and follow-up visual acuity measurements were not obtained systematically. However, the strengths of this study were that it was a single-surgeon, consecutive case series study conducted over a 10-year period in which all patients were postoperatively observed for at least 24 months by the operating surgeon.
In conclusion, the anatomical success rate of LSV after a mean follow-up period of 5.6 years was found to be encouraging for the correction of TRD associated with stage 4B ROP but not for stage 5 ROP. Although the long-term visual outcomes were not satisfactory, favorable outcomes were obtained in cases in which the retinas were reattached. In addition, complications developed frequently after longer follow-up periods, especially in eyes with persistent TRD. Therefore, the ultimate goal of LSV in the treatment of TRD associated with ROP is to attain retinal reattachment, which is important for obtaining better visual outcomes and preventing the development of late complications; LSV may be an effective treatment option for TRD associated with ROP.
REFERENCES
1. Gilbert WS, Quinn GE, Dobson V, et al. Multicenter Trial of Cryotherapy for Retinopathy of Prematurity Cooperative Group. Partial retinal detachment at 3 months after threshold retinopathy of prematurity. Long-term structural and functional outcome. Arch Ophthalmol 1996;114:1085-1091.


2. Cryotherapy for Retinopathy of Prematurity Cooperative Group. Multicenter trial of cryotherapy for retinopathy of prematurity: ophthalmological outcomes at 10 years. Arch Ophthalmol 2001;119:1110-1118.


3. Greven C, Tasman W. Scleral buckling in stages 4B and 5 retinopathy of prematurity. Ophthalmology 1990;97:817-820.


4. Noorily SW, Small K, de Juan E Jr, Machemer R. Scleral buckling surgery for stage 4B retinopathy of prematurity. Ophthalmology 1992;99:263-268.


6. Hinz BJ, de Juan E Jr, Repka MX. Scleral buckling surgery for active stage 4A retinopathy of prematurity. Ophthalmology 1998;105:1827-1830.


7. Machemer R. Closed vitrectomy for severe retrolental fibroplasia in the infant. Ophthalmology 1983;90:436-441.


8. Chong LP, Machemer R, de Juan E. Vitrectomy for advanced stages of retinopathy of prematurity. Am J Ophthalmol 1986;102:710-716.


9. Trese MT, Droste PJ. Long-term postoperative results of a consecutive series of stages 4 and 5 retinopathy of prematurity. Ophthalmology 1998;105:992-997.


10. Capone A Jr, Trese MT. Lens-sparing vitreous surgery for tractional stage 4A retinopathy of prematurity retinal detachments. Ophthalmology 2001;108:2068-2070.


11. Moshfeghi AA, Awner S, Salam GA, Ferrone PJ. Excellent visual outcome and reversal of dragging after lens sparing vitrectomy for progressive tractional stage 4a retinopathy of prematurity retinal detachment. Retina 2004;24:615-616.


12. Hartnett ME, Maguluri S, Thompson HW, McColm JR. Comparison of retinal outcomes after scleral buckle or lens-sparing vitrectomy for stage 4 retinopathy of prematurity. Retina 2004;24:753-757.


13. Prenner JL, Capone A Jr, Trese MT. Visual outcomes after lens-sparing vitrectomy for stage 4A retinopathy of prematurity. Ophthalmology 2004;111:2271-2273.


14. Hubbard GB 3rd, Cherwick DH, Burian G. Lens-sparing vitrectomy for stage 4 retinopathy of prematurity. Ophthalmology 2004;111:2274-2277.


15. Moshfeghi AA, Banach MJ, Salam GA, Ferrone PJ. Lens-sparing vitrectomy for progressive tractional retinal detachments associated with stage 4A retinopathy of prematurity. Arch Ophthalmol 2004;122:1816-1818.


16. Lakhanpal RR, Sun RL, Albini TA, Holz ER. Anatomic success rate after 3-port lens-sparing vitrectomy in stage 4A or 4B retinopathy of prematurity. Ophthalmology 2005;112:1569-1573.


17. Lakhanpal RR, Davis GH, Sun RL, et al. Lens clarity after 3-port lens-sparing vitrectomy in stage 4A and 4B retinal detachments secondary to retinopathy of prematurity. Arch Ophthalmol 2006;124:20-23.


18. Lakhanpal RR, Sun RL, Albini TA, et al. Visual outcomes after 3-port lens-sparing vitrectomy in stage 4 retinopathy of prematurity. Arch Ophthalmol 2006;124:675-679.


19. Yu YS, Kim SJ, Kim SY, et al. Lens-sparing vitrectomy for stage 4 and stage 5 retinopathy of prematurity. Korean J Ophthalmol 2006;20:113-117.



20. Lakhanpal RR, Sun RL, Albini TA, Holz ER. Anatomical success rate after primary three-port lens-sparing vitrectomy in stage 5 retinopathy of prematurity. Retina 2006;26:724-728.


21. Micelli Ferrari T, Furino C, Lorusso VV, et al. Three-port lens-sparing vitrectomy for aggressive posterior retinopathy of prematurity: early surgery before tractional retinal detachment appearance. Eur J Ophthalmol 2007;17:785-789.


22. El Rayes EN, Vinekar A, Capone A Jr. Three-year anatomic and visual outcomes after vitrectomy for stage 4B retinopathy of prematurity. Retina 2008;28:568-572.


23. Bhende P, Gopal L, Sharma T, et al. Functional and anatomical outcomes after primary lens-sparing pars plana vitrectomy for stage 4 retinopathy of prematurity. Indian J Ophthalmol 2009;57:267-271.



24. Azuma N, Ishikawa K, Hama Y, et al. Early vitreous surgery for aggressive posterior retinopathy of prematurity. Am J Ophthalmol 2006;142:636-643.


25. Kondo H, Arita N, Osato M, et al. Late recurrence of retinal detachment following successful vitreous surgery for stages 4B and 5 retinopathy of prematurity. Am J Ophthalmol 2009;147:661-666.e1.


26. The International Committee for the Classification of the Late Stages of Retinopathy of Prematurity. An international classification of retinopathy of prematurity. II. The classification of retinal detachment. Arch Ophthalmol 1987;105:906-912.


27. Maguire AM, Trese MT. Lens-sparing vitreoretinal surgery in infants. Arch Ophthalmol 1992;110:284-286.


28. Hartnett ME. Features associated with surgical outcome in patients with stages 4 and 5 retinopathy of prematurity. Retina 2003;23:322-329.


29. Chuang YC, Yang CM. Scleral buckling for stage 4 retinopathy of prematurity. Ophthalmic Surg Lasers 2000;31:374-379.


30. Ricci B, Santo A, Ricci F, et al. Scleral buckling surgery in stage 4 retinopathy of prematurity. Graefes Arch Clin Exp Ophthalmol 1996;234(Suppl 1):S38-S41.


Table 2
Patient's demographics and outcomes
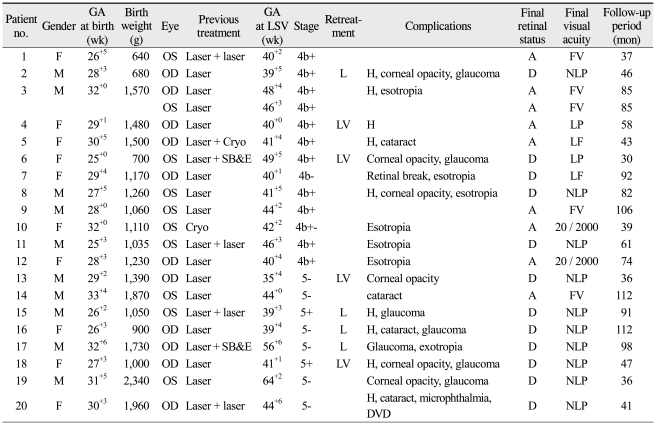
GA = gestational age; LSV = lens sparing vitrectomy; F = female; M = male; OD = right eye; OS = left eye; Cryo = cryotherapy; SB&E = scleral buckling and encircling; L = lensectomy; LV = lensectomy and additional vitrectomy; H = postoperative intraocular hemorrhage; DVD = dissociated vertical deviation; A = attached; D = detached; NLP = no light perception; LF = light follow; LP = light perception; FV = form vision; - = plus absent; + = plus present; +- = plus trace




 PDF Links
PDF Links PubReader
PubReader Full text via DOI
Full text via DOI Full text via PMC
Full text via PMC Download Citation
Download Citation Print
Print




