 |
 |
| Korean J Ophthalmol > Volume 24(2); 2010 > Article |
Abstract
Here we report a case of optic neuritis in the setting of herpes zoster ophthalmicus (HZO) in a child. A six-year-old girl presented with HZO in the right eye. During the hospitalization, her visual acuity decreased. Fluorescein angiography (FAG) and optical coherence tomography revealed optic neuritis in the affected eye. Visual acuity improved with one month of treatment with acyclovir and steroids. FAG analysis showed no evidence of leakage at the optic disc. At one year post treatment, the patient's fundus exam and vision were normal. Therapy with antivirals and steroids may be effective in patients with childhood HZO optic neuritis.
Herpes zoster is an infectious disease that results from the reactivation of a latent varicella zoster virus (VZV) in individuals who have had varicella (chickenpox) sometime within their lifespan [1]. Herpes zoster ophthalmicus (HZO) involves the ophthalmic branch of the trigeminal nerve by recurrent VZV infection, and may lead to severe pain and a wide spectrum of sight-threatening complications [2] affecting all ocular and orbital tissues [3]. The ophthalmic division of the trigeminal nerve is involved in 8% [4] to 56% [5] of all herpes zoster infections.
The most common ocular findings in adult patients with HZO include conjunctivitis, keratitis, uveitis, and secondary glaucoma. However, optic neuritis is an uncommon complication of HZO. Since it was first described by Hutchinson in 1866 [6], several reports have described HZO optic neuritis that lead to optic atrophy [7], retrobulbar neuritis, or papillitis [8].
HZO is rare in children and, when it does occur, it tends to run a shorter, more benign course than that observed in adults [9]. Only one case has been reported where HZO optic neuritis occurred in a child, and the resulting final visual acuity was not improved following resolution of the infection [10]. However, in the current study, the patient experienced a good clinical outcome.
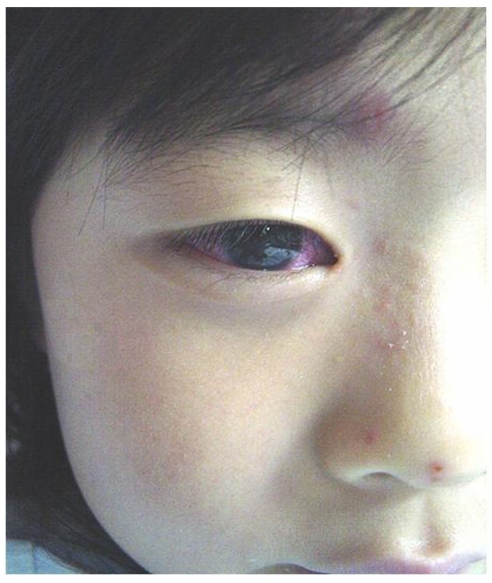
A six-year-old girl presented to the Pediatric Department at Wonkwang University hospital with the chief complaint of mild fever, hyperemic conjunctiva, and a skin rash over the right side of her forehead (Fig. 1). She was diagnosed with Herpes zoster and admitted to the pediatric department. There were no significant findings in laboratory testing. She was administered intravenous acyclovir (250 mg) every eight hours and antibiotics (a third generation cephalosporin, 500 mg) every 12 hours for five days.
The day after admission, a consult for ophthalmic evaluation was requested due to the erythematous eye. External findings included the characteristic maculopapular rash involving the entire distribution area of the right trigeminal nerve. She complained of decreased vision in the right eye; however, visual acuity was 0.8 (OD)/1.0 (OS). Slit lamp examination revealed many inflammatory cells in the anterior chamber but a quiet fundus in the right eye. There was no marked sign of a relative afferent pupillary defect. The patient was diagnosed with an anterior uveitis and was treated with topical steroids (0.12% prednisolone) and cycloplegic drops six times per day.
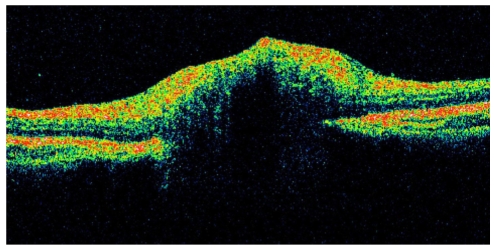
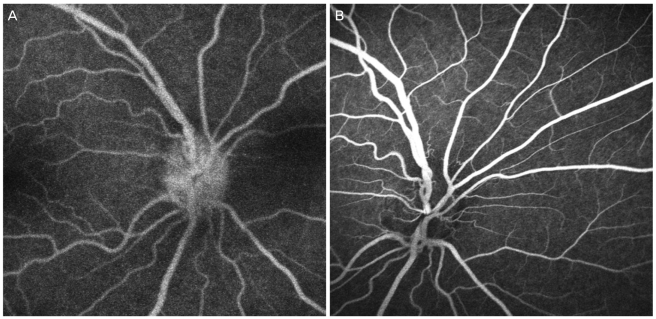
Two days later the cornea presented with Descemet's membrane folding and keratic precipitates distributed evenly across the corneal endothelium. One week after the first visit, the patient returned with reduced visual acuity in the right eye. Her visual acuity was 0.4, and the intraocular pressure was 6 mmHg in the affected eye. There were still many inflammatory cells in the anterior chamber. Examination of the fundus demonstrated mild edema, congestion of the optic Coherence Tomography (OCT) (Fig. 2). Fluorescein angiography (FAG) revealed hyperfluorescence in the optic disc, and this was increased in the later phase with normal retinal circulation (Fig. 3A). Visual field testing could not be obtained due to a lack of patient's cooperation. A Brain MRI was performed, and it demonstrated no acute pathology. Based on these findings, the patient was diagnosed with HZO optic neuritis.
The antiviral agent was switched to oral acyclovir (250 mg) every eight hours for ten days, and oral prednisolone (20 mg) was added once a day for ten days following discharge. At a one month follow-up visit, her visual acuity had recovered to 0.8 (OD). Her external exam was also improved. Hyperfluorescence and swelling of the optic disc had resolved, as revealed by follow-up FAG (Fig. 3B). At a one year follow-up visit, the patient's visual acuity and fundus examination were normal.
Herpes zoster virus involves the ophthalmic branch of the trigeminal nerve by recurrence of virus that has persisted in the sensory nerve ganglia [11] in a latent form. The virus produces herpes zoster with a typical vesicular rash in the distribution of one or more cutaneous dermatomes [12]. Decreased cellular immunity is likely the leading cause of VZV reactivation, while humoral immunity remains intact in most patients [1].
Varicella often occurs in childhood, whereas zoster is most commonly seen among the elderly who have a less robust cell-mediated immune response associated with advancing age [11]. Because of this, herpes zoster is not common in children; however, it can occur when a child has experienced varicella infection prior to one year of age [13]. The interval between varicella infection and childhood zoster averages 3.8 years if varicella infection occurs during the first year of life, but averages 6.2 years if infection occurs after the age of one year [14].
In the present case, the patient has not had a known varicella infection; the patient did receive a vaccination against varicella at one year of age. The overall incidence of herpes zoster in children who have received varicella vaccination is low compared to that of children who have had a varicella infection [15].
HZO may lead to severe pain and a wide spectrum of sight-threatening complications affecting all ocular and orbital tissues [3]. These sequela are caused by nerve damage, chronic inflammation, or by direct viral infection [16]. HZO with ocular involvement is relatively common in adults, accounting for 10-25% of all cases of herpes zoster [17]. However, HZO is rarely found in children, having an incidence of 0.42% [15]. When HZO occurs in children, it tends to run a shorter, more benign course than that seen in adults [9].
Optic nerve involvement is a very rare sequelae of childhood HZO; to date, only one previous case [18] has been reported. In comparison, optic nerve involvement of HZO in adults has been frequently reported. This condition may present as papillitis, optic neuritis, or optic nerve infarction [19]. Optic neuritis following HZO appears weeks to months after the onset of skin lesions, and loss of visual acuity varies from severe bilateral impairment to moderate unilateral impairment [20].
The final confirmation of VZV optic neuritis depends on clinical findings and the exclusion of other etiologies, as pathologic examination of the optic nerve cannot be performed [20]. As to the pathogenesis of the optic neuritis, VZV produces inflammation in the posterior root ganglia and the ganglia of certain cranial nerves, such as the gasserian ganglion. Inflammation commonly extends down from the gasserian ganglion to the ophthalmic division of the trigeminal nerve. The exact mechanism(s) by which herpes zoster produces optic neuritis is unclear. However, the optic nerve may be involved by the following three mechanisms:
(1) Direct extension of the virus through the cavernous sinus to nerves, muscles, and the optic nerve [19].
(2) Local extension into the meninges and brain tissue may lead to mild meningoencephalitis, which, in turn, may damage the optic nerve [19,21].
(3) Generalized ocular ischemia caused by inflammation [19].
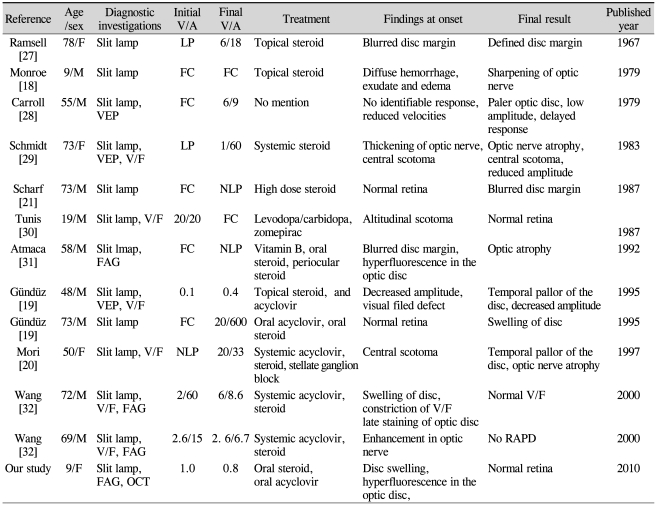
In the current case, the optic neuritis was demonstrated by hyperfluorescence of the optic disc and normal retinal circulation by FAG, disk elevation by OCT, and swelling of the optic disc as seen by slit lamp examination. Unfortunately, a visual field test could not be obtained secondary to the patient's age and inability to cooperate with the exam. Visual outcomes are usually poor in the setting of optic neuropathy resulting from HZO [19] when steroids are used as monotherapy (Table 1). Following the administration of antiviral agents, such as acyclovir, visual acuity generally improves. In the current case, visual acuity improved following oral acyclovir and steroid administrations. The use of high-dose systemic antiviral agents has been reported to be beneficial in these patients, reducing the severity and duration of ocular inflammation caused by HZO [22].
Acyclovir has been the drug of choice for the treatment of herpes zoster infection. The recommended dosage for acyclovir is 5-10 mg/kg intravenously every eight hours [23]. Famciclovir or valacyclovir are dosed less frequently, have better bioavailability, and are superior in terms of compliance and inhibition of postherpetic neuralgia in adults, but these substances are not approved for the pediatric population [24].
Most sources advocate the treatment of zoster-related optic neuritis with systemic steroids and claim a good clinical response with this treatment [25]. Patients receiving steroids have been shown to have a moderate, but statistically significant, acceleration in the rate of cutaneous healing and alleviation of acute pain. Systemic steroids improve the quality of life, but should not be used in patients with contraindications [26]. Although the VZV vaccine is relatively effective in preventing chickenpox in children, infections can still occur [10].
Here we reported the case of a young girl with optic neuritis experienced during the course of HZO. Prompt treatment with steroids and antiviral agents may improve the final visual outcome in similar cases.
REFERENCES
1. Weller TH. Varicella and herpes zoster: changing concept of the natural history, control, and importance of a not-so-benign virus. N Engl J Med 1983;309:1362-1368.


2. Pavan-Langston D. In: Foster CS, Azar D, Dohlman CH, Viral disease of the ocular anterior segment: basic science and clinical disease. The cornea. 2005. Philadelphia: Lippincott Williams & Wilkins; p. 297-397.

3. Culbertson WW, Blemenkranz MS, Pepose JS, et al. varicella zoster virus is a cause of the acute retinal necrosis syndrome. Ophthalmology 1986;93:559-569.


4. Hope-Simpson RE. The nature of herpes zoster: a long term study and a new hypothesis. Proc R Soc Med 1965;58:9-20.



5. Juel-Jensen BE, MacCallum FO. Herpes simplex varicella and zoster. 1972. Philadelphia: Lippincott; p. 109.
6. Kattah JC, Kennerdell JS. Orbital apex syndrome secondary to herpes zoster ophthalmicus. Am J Ophthalmol 1978;85:378-382.


8. Hamard H, Chevaleraud J, Rondot P. Neuropathies optiques Inflammatoires et infectieuses. Neuropathies optiques. 1986. Paris: Masson; p. 281.
9. Edgerton AE. Herpes zoster ophthalmicus: report of cases and review of literature. Arch Ophthal 1945;34:114-153.

10. Liang MG, Heidelberg KA, Jacobson RM, McEvoy MT. Herpes zoster after varicella immunization. J Am Acad Dermatol 1998;38:761-763.


11. Straus SE, Reinhold W, Smith HA, et al. Endonuclease analysis of viral DNA from varicella and subsequent zoster infections in the same patient. N Engl J Med 1984;311:1362-1364.


12. Burke BL, Steele RW, Beard OW, et al. Immune responses to varicella-zoster in the aged. Arch Intern Med 1982;142:291-293.


13. Baba K, Yabuuchi H, Takahashi M, Ogra PL. Increased incidence of herpes zoster in normal children infected with varicella zoster virus during infancy: community-based follow-up study. J Pediatr 1986;108:372-377.


15. Uebe B, Sauerbrei A, Burdach S, Horneff G. Herpes zoster by reactivated vaccine varicella zoster virus in a healthy child. Eur J Pediatr 2002;161:442-444.


16. Gilden DH, Cohrs RJ, Mahalingam R. VZV vasculopathy and postherpetic neuralgia: progress and perspective on antiviral therapy. Neurology 2005;64:21-25.


17. Shaikh S, Ta CN. Evaluation and management of herpes zoster ophthalmicus. Am Fam Physician 2002;66:1723-1730.

19. G├╝nd├╝z K, Ozdemir O. Bilateral retrobulbar neuritis following unilateral herpes zoster ophthalmicus. Ophthalmologica 1994;208:61-64.


20. Mori T, Terai T, Hatano M, et al. Stellate ganglion block improved loss of visual acuity caused by retrobulbar optic neuritis after herpes zoster. Anesth Analg 1997;85:870-871.


21. Scharf Y, Kraus E, Zonis S. Optic neuropathy and central retinal artery occlusion in a case of herpes zoster ophthalmicus. Ann Ophthalmol 1987;19:77-78.

22. Tyring S, Engst R, Corriveau C, et al. Famciclovir for ophthalmic zoster: a randomized aciclovir controlled study. Br J Ophthalmol 2001;85:576-581.



24. Davis LE, King MK. Shingles (herpes zoster) and post-herpetic neuralgia. Curr Treat Options Neurol 2001;3:401-411.


26. Wood MJ, Johnson RW, McKendrick MW, et al. A randomized trial of acyclovir for 7 days or 21 days with and without prednisolone for treatment of acute herpes zoster. N Engl J Med 1994;330:896-900.


28. Caroll WM, Mastaglia FL. Optic neuropathy and ophthalmoplegia in herpes zoster oticus. Neurology 1979;29:726-729.


29. Schmidt P. Herpes zoster ophthalmicus with retrobulbar neuritis. A case report. Acta Ophthalmol 1983;61:501-509.
30. Tunis SW, Tapert MJ. Acute retrobulbar neuritis complicating herpes zoster ophthalmicus. Ann Ophthalmol 1987;19:453-456.




 PDF Links
PDF Links PubReader
PubReader Full text via DOI
Full text via DOI Full text via PMC
Full text via PMC Download Citation
Download Citation Print
Print




