 |
 |
| Korean J Ophthalmol > Volume 37(3); 2023 > Article |
|
Abstract
Purpose
To evaluate the effect of intraoperative mitomycin C (MMC) on the surgical outcomes of ciliary sulcus (CS) Ahmed glaucoma valve (AGV) tube placement.
Methods
A retrospective review of medical records of 54 consecutive patients who underwent AGV implantation with tube placed in CS was performed. Consecutive cases operated without the use of intraoperative MMC from 2017 to 2019 were compared with consecutive cases operated with MMC from 2019 to 2021. Surgical failure was defined as intraocular pressure (IOP) exceeding 21 mmHg in two consecutive visits after postoperative 3 months or Ōēż30% IOP reduction, IOP Ōēż5 mmHg in two consecutive visits, or loss of light perception. Kaplan-Meier survival analysis and log-rank test were performed to compare the surgical failure rates.
Results
A total of 54 eyes of 54 patients were investigated. Mean follow-up period after AGV implantation was 1.4 ┬▒ 0.8 years. The MMC group showed significantly lower IOP during the 1st postoperative month (20.5 ┬▒ 8.6 mmHg vs. 15.8 ┬▒ 6.4 mmHg, p = 0.027), but the difference did not persist 6 months after the surgery (p = 0.805). The mean number of postoperative antiglaucoma medications was significantly lower in the MMC group in the 1st postoperative month (p = 0.047) but no difference was found at 6 months. No statistical difference was noted in the rates of postoperative complications. Kaplan-Meier survival analysis showed comparable survival rates between MMC group and no MMC group (p = 0.356).
Glaucoma drainage devices (GDD) are becoming one of the most preferred surgical methods to control intraocular pressure (IOP) especially in refractory glaucoma [1,2]. Previous clinical trials have demonstrated similar IOP reducing effect and better surgical success rate of GDD to that of trabeculectomy [3]. Comparable success rate and fewer early complications have increased its popularity in the management of glaucoma [4]. However, the use of GDD is hampered by two main drawbacks. First, success rates fall with time in part because of the development of fibrotic pseudocapsule around the valve plate that resists aqueous flow [5]. Second, its presence has been associated with long-term corneal endothelial cell damage [6].
Considerable efforts have been made to address these drawbacks. For instance, instead of anterior chamber (AC), tube placement into ciliary sulcus (CS) has been attempted by a number of groups to further increase the distance between the corneal endothelium and the possible irritant [6-10]. So far, results have been promising. Slower rates of endothelial damage and comparable IOP reduction have been reported [6,8]. As for pseudocapsule development, antifibrotic agents, which have already been widely used in trabeculectomy, has been adopted both during and after surgery to decrease fibrosis and improve bleb function. Randomized clinical trials have failed to justify its use for long-term success [11], but a number of retrospective studies have hinted that the use of antifibrotic agents like mitomycin C (MMC) might improve IOP control at least early in the postoperative period [12,13].
So far, the evaluation of the effect of antifibrotic agents in Ahmed glaucoma valve (AGV) implantation has been limited to cases where valve tube was positioned in AC [11-13]. As AGV tube placed in CS showed comparable IOP reduction effect and surgical failure rate compared to AGV tube placed in AC during short-term follow-up [8], the effect of adjunctive use of antifibrotic agent on AGV tube placed in CS also needs to be analyzed along the post-operative progress. Therefore, in this study, we compared the surgical outcome of AGV implantation in which tube was positioned in CS according to the use of MMC during surgery.
The study adhered to the tenets of the Declaration of Helsinki and the protocol was approved by the Institutional Review Board of Yonsei University Severance Hospital (No. 4-2021-1501). Written informed consent was waived due to the retrospective nature of the study.
A retrospective review of medical records was performed to evaluate patients who received AGV model FP7 implantation during which the tube was placed in CS during the period from March 2017 to January 2021. All patients with uncontrolled glaucoma on maximum tolerated medical therapy with at least 6 months of postoperative follow-up were considered eligible.
Exclusion criteria were as follows: (1) patients <18 years of age; (2) concomitant surgery such as cataract extraction or vitrectomy; (3) previous AGV implantation in the same eye; (4) history of corneal graft transplantation; (5) history of corneal refractive surgery; (6) history of ocular trauma; (7) preoperative visual acuity worse than hand motion; (8) aphakia; (9) signs of vitreous prolapse into AC; (10) congenital glaucoma; (11) suspicion of steroid-induced glaucoma; and (12) previous vitrectomy. Only one eye per patient was included for our study. When both eyes were eligible, only the first operated eye was included. All consecutive eyes that underwent AGV implantation between March 2017 and April 2019 were operated without the use of MMC. All AGV implantations performed between July 2019 and January 2021 involved the application of MMC during the surgery.
A detailed description of the surgical procedure is provided elsewhere [6]. All surgeries were performed under local anesthesia. A 6-0 silk traction suture was placed under the insertion of the superior recuts muscle to retract eyeball downward to achieve optimal exposure of the superotemporal quadrant of conjunctiva. Fornix-based conjunctival incision was made, and Tenon capsule was dissected using spring scissors. A 4 ├Ś 4-mm right angled triangular of partial thickness and a 2 ├Ś 6-mm bridge shaped flap of partial thickness were made on the sclera of the superotemporal quadrant. In patients who received intraoperative MMC, a large weck-cell sponge soaked in a 0.5 mg/mL solution of MMC was placed on the episcleral for a contact time of 5 minutes, followed by irrigation with 30 mL of balanced salt solution (BSS). The remainder of surgical procedure was identical for both groups. The tube was primed with BSS, and the anterior edge of the AGV plate was positioned at least 8 mm from the limbus. A 23-gauge needle tract was made 2 to 3 mm posterior to the limbus under the scleral flap to advance the tube into the CS in a bevel-down fashion. The scleral flaps were positioned over the tube and sutured with 10-0 nylon. Conjunctiva and Tenon capsule was sutured near the limbus with interrupted 8-0 vicryl sutures.
The postoperative regimen included a topical antibiotics and topical steroids for 1 month. Topical corticosteroids were started at every 2 hours or four times a day at the attending physicianŌĆÖs discretion and tapered for a period of 1 month. No standardized protocol was devised to determine the IOP threshold or the type of glaucoma medications started during the postoperative management. Medications were added as necessary to further reduce IOP and its type was determined based on previous glaucoma medications, allergy history and cost at the attending physiciansŌĆÖ discretion. Patients were examined 1 day, 1 week, 1 month, 3 months, and 6 months after the surgery.
Records of IOP, number of antiglaucoma medications and the presence of any complications during postoperative follow-up were collected. Hypertensive phase was defined as IOP exceeding 21 mmHg within the first three postoperative months following initial IOP reduction to below 22 mmHg in the 1st week postoperation, not caused by tube obstruction, retraction, or valve malfunction [13]. Surgical failure was defined as IOP exceeding 21 mmHg in two consecutive visits after postoperative 3 months or Ōēż30% IOP reduction relative to preoperative values; IOP Ōēż5 mmHg in two consecutive visits; or loss of light perception. Eyes requiring additional glaucoma surgery or developing phthisis were also considered failures [11]. IOP reduction was calculated as the difference between follow-up IOP and preoperative IOP divided by the preoperative IOP values.
Continuous variable was presented as mean ┬▒ standard deviation and categorical variable was presented as number (percentage). Assessment of normality was conducted using the Shapiro-Wilk test. Continuous variable was compared using Student t-test, and categorical variable was compared using chi-square test and Fisher exact test between no MMC and MMC groups. Surgical failure rates were compared using Kaplan-Meier survival analysis and log-rank test. All mentioned analyses were conducted using R ver. 4.1.1 (R Foundation for Statistical Computing). A p-value of <0.05 was considered as statistically significant.
A total of 54 eyes underwent implantation of AGV model FP7 with tube placed in CS for uncontrolled glaucoma on maximum tolerated medical therapy. Of them, 22 eyes were operated between March 2017 and April 2019 without the use of intraoperative MMC and were designated the no MMC group (mean age, 65.2 ┬▒ 13.1 years; male patient, 59.1%). Six of the 22 eyes were operated by HWB and the rest were operated by CYK. The 32 eyes of the MMC groups are those operated between June 2019 and January 2021 using MMC (mean age, 67.6 ┬▒ 14.1 years; male patient, 56.3%) by a single surgeon (CYK).
All 22 eyes of the no MMC group and 18 of the MMC group completed 1 year follow-up. Comparisons of baseline characteristics between the two groups are illustrated in Table 1. The mean age (p = 0.532) and sex distribution (p = 0.999) were comparable between the two groups. No statistical difference was noted in the types of glaucoma (p = 0.789) or the severity of glaucoma (retinal nerve fiber layer thickness, p = 0.968; visual field mean deviation, p = 0.681).
Comparisons of average IOP between the two groups during follow-up are shown in Table 2. The mean preoperative IOP was comparable (26.8 ┬▒ 8.0 mmHg vs. 27.2 ┬▒ 8.0 mmHg, p = 0.857). Both groups showed IOP reduction following AGV tube placement in CS on the 1st week after surgery (10.8 ┬▒ 4.8 mmHg vs. 11.6 ┬▒ 7.1 mmHg). The average IOP was significantly lower in the MMC group in the 1st postoperative month (20.5 ┬▒ 8.6 mmHg vs. 15.8 ┬▒ 6.4 mmHg, p = 0.027), but significant difference in IOP was not observed in the remainder of the follow-up period until 6 months (p > 0.05). Hypertensive phases were observed in 14 out of 22 eyes (63.6%) in the no MMC group and 11 out of 32 eyes (34.4%) in the MMC group, but the difference was not statistically significant (p = 0.066). When the number of antiglaucoma medications required were compared (Table 3), the number of medications at preoperation was comparable (p = 0.062). Neither group required the use of antiglaucoma medications in the 1st week following AGV implantation. However, the no MMC group were on a significantly greater number of medications by the 1st postoperative month (1.4 ┬▒ 0.9 vs. 0.8 ┬▒ 1.0, p = 0.047). For the rest of the follow-up period up until 6 months, the number of antiglaucoma medications was comparable for the two groups. Mean IOP (16.0 ┬▒ 5.9 mmHg vs. 14.9 ┬▒ 3.9 mmHg) and postoperative antiglaucoma medication (1.8 ┬▒ 0.8 vs 1.7 ┬▒ 1.0) also did not show significant difference at postoperative 1 year between MMC group and no MMC group; however, further investigations are necessary for 1-year results due to varying dropout rates between them after postoperative 6 months.
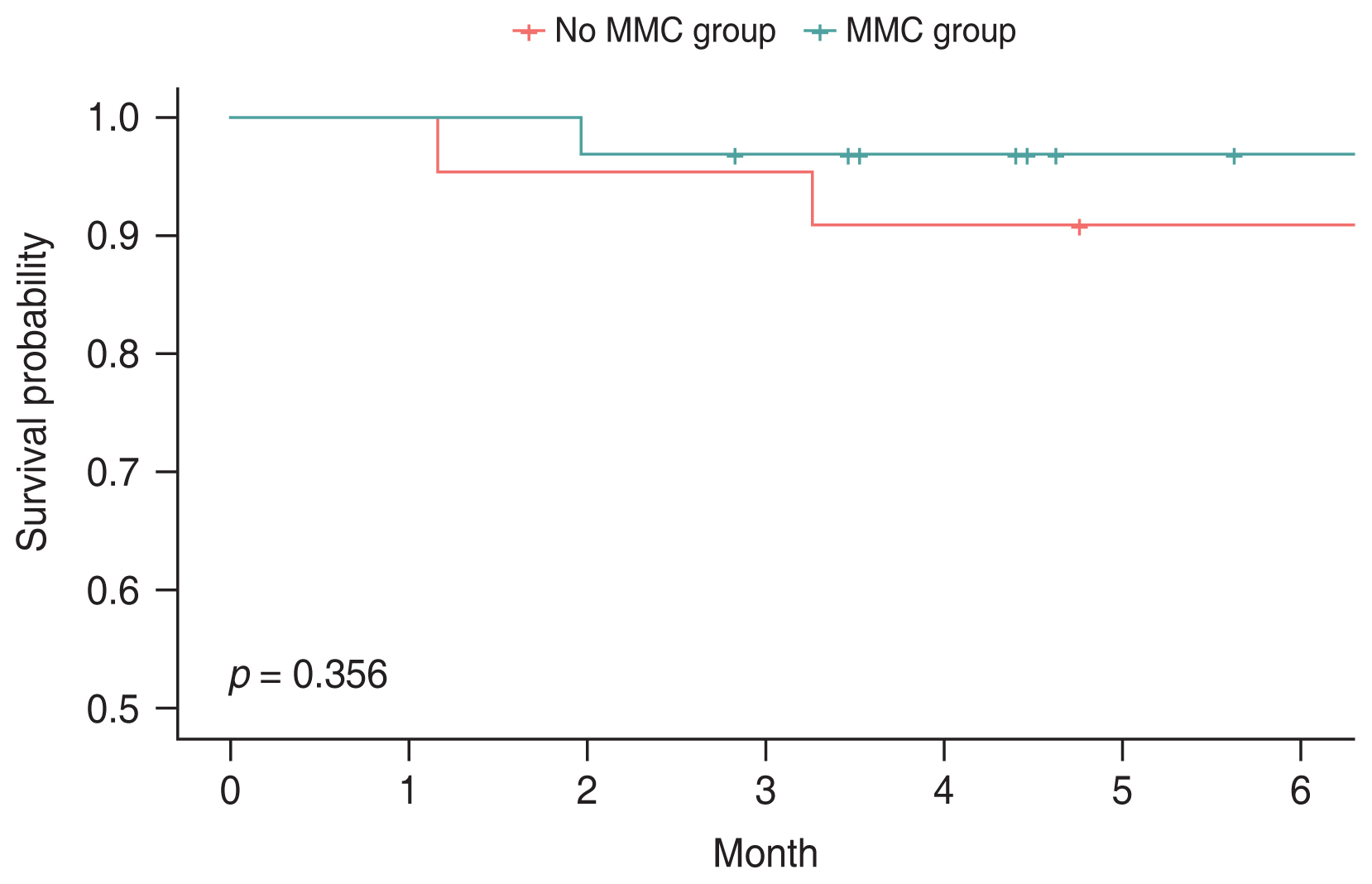
The 6-month survival probabilities were 96.8% for MMC group and 91.0% for no MMC group. Kaplan-Meier survival analysis was conducted to compare surgical failure rates (Fig. 1), no significant difference was noted (p = 0.356 by log-rank test).
Postoperative complications are listed in Table 4. Hyphema was the most common complication following AGV tube placement in CS. Peritubular leakage was noted in one patient belonging to the MMC group (p = 0.999). Flat AC was observed in one patient from each group (p = 0.999). The rates of postoperative complications were not significantly different between the two groups.
In the present study, we compared the surgical outcome of patients who underwent CS AGV implantation depending on the intraoperative application of MMC. According to our analysis, while the average IOP was significantly lower in the group of patients who received intraoperative MMC in the first postoperative month, no significant difference was found 6 months after surgery. The use of MMC did not increase rates of postoperative complications. To the best of our knowledge, our study is the first to evaluate the effect of intraoperative MMC in patients who underwent AGV implantation with the tube placed in CS.
The average IOP of the study population of the present study was comparable to those reported by prior studies on CS AGV. Eslami et al. [9] reported that the mean IOP was 16.2 ┬▒ 3.6 mmHg at 1 year. Bayer and Onol [8] similarly reported that the patients who received AGV in CS showed IOP of 14.4 ┬▒ 6.8 mmHg. The report by Arikan et al. [7] also presented that the average IOP at 1 year was 15.6 ┬▒ 5.4 mmHg. In terms of IOP at 1 month, however, previous studies mentioned above vary widely, preventing direct comparisons to the results of our study. Eslami et al. [9] demonstrated that the average IOP 1 month postoperation was approximately 20 mmHg in their patient population, a value similar to that of the no MMC group of the present study. In contrast, Bayer and Onol [8] and Arikan et al. [7] showed that the IOP was in the range between 10 and 15 mmHg, which is more comparable to the 1-month result of our MMC group. The variations from those reported in the literature may be due to a number of factors, including the ethnic characteristics, preoperative IOP and candidate selection for AGV implantation [14,15].
The benefits of intraoperative MMC were similar to previous reports that tested the effect of intraoperative use of antifibrotic agents in AC AGV implantation. A randomize clinical trial conducted by Costa et al. [11] showed that the MMC group benefitted from the antifibrotic agents by demonstrating significantly lower IOP in the early periods of follow-up, 7th, and 15th days after surgery, in comparison to the control [11]. However, the difference did not remain significant at 1 year of follow-up. Despite different tube location, the results of our analysis were generally in line with the previous study; the average IOP of the MMC group in the present study was significantly lower in the 1st operative month, but the benefits did not persist 6 months after the implantation. Although the clinical trial did not support the use of MMC for improved success rates of AGV, we believe that the decrease in IOP in the 1st postoperative month, during which AGV is generally associated with hypertensive phase, is worth noting. Experiencing a hypertensive phase has previously been described as a risk factor for valve failure [16-18]. Other studies investigating the effect of antifibrotic agents have emphasized the importance of attenuating the hypertensive phase in patients who received AGV implantation. For example, a recent report by Perez et al. [13] subjected patients to intraoperative and postoperative subconjunctival MMC injections in order to reduce the incidence of hypertensive phase (defined as IOP exceeding 21 mmHg during the first three postoperative months) among patients who underwent AC AGV implantation. Other studies have also highlighted the role of antifibrotic agents in reducing incidences of hypertensive phases in the past [12,19,20]. Even though the MMC group of the present study showed significantly lower IOP in the 1st postoperative month, when the definition of the hypertensive phase was adopted as mentioned above to calculate its rate in the two groups, no significant difference was noted (p = 0.062). We propose the following explanations for this result. First, events of IOP exceeding 21 mmHg in a patient population, whose preoperative IOP might be relatively low due to a higher prevalence of normal tension glaucoma, may be rarer. Second, aggressive use of antiglaucoma medications to control IOP in the 1st postoperative month in expectation of hypertensive phase may have decreased its incidence at 3 months postoperation. Third, the slight difference may not have been detected due to a relatively small sample size. Whether any form of attenuation of IOP early in the follow-up produces differences in terms of AGV failure or disease progression further along the course of the disease needs to be investigated in depth by future studies.
The little disparities between results of our study from previous investigations with AC AGV were somewhat unexpected. MMC applied during surgery is on one hand expected to inhibit fibrovascular reaction to reduce encapsulation around the plate during early phases of postoperative period, thereby attenuating hypertensive phase usually between 1st and 3rd postoperative months [21]. The inhibitory effect is thought to be eventually overcome by the presence of a foreign body that constantly triggers fibroelastic wound healing response, resulting in little difference in the long-term [22]. However, an alternative explanation offered by previous studies on fluctuations of IOP during postoperative period in eyes exposed to intraoperative MMC were toxic effect of the antifibrotic agent on the ciliary body epithelium [11,23,24]. Consequent inflammation and reduced aqueous humor production might contribute to reduction of IOP, which eventually increase with the resolution of inflammation. In this regard, we speculated that these effects of MMC on inflammation, if present, may differ when the tube is placed in CS instead of AC. The tube may cause direct mechanical damage to the ciliary body when inserted in the CS to decrease aqueous humor production [8,10]. The tube in CS has also been associated with greater incidences of iris tenting, and contact with the iris may result in greater degrees of postoperative inflammation [6,25]. Furthermore, a longer tunnel (sclera and ciliary body tissues) may make tubes in CS more vulnerable to rise in IOP by fibrotic changes around the plate in comparison to tube in AC (sclera). Our comparisons among patients receiving CS AGV did not follow our expectations as the effect of MMC on IOP was generally similar to that reported by other studies on AC AGV. Our analysis also showed that intraoperative MMC did not increase the postoperative complication rates among patients receiving CS AGV. Previous clinical trials as well as retrospective studies on AC AGV also noted comparable complication rates [11-13]. We do not have clear explanations for the similarities between AC AGV and CS AGV. We speculate that our surgical technique of brief contact between episclera and the antifibrotic agent instead of subconjunctival injection might have resulted in minimal exposure of ciliary body epithelium to MMC. It is also possible that the impact of fibrotic changes around the plate on IOP were too substantial relative to that of the tube location, masking any differences that might have existed. However, because our study did not directly compare AC AGV and CS AGV, future investigations are necessary to identify if any differences exist in valve function in eyes exposed to antifibrotic agents depending on the tube location. There were several limitations to the present study. First, the study is limited by its retrospective design. Second, no single protocol was adopted for the management of patients. Although the majority patients underwent operations by a single surgeon, inclusion of cases performed by more than one surgeon produced variations in terms of patient selection, surgical technique and postoperative management.
Third, patients were observed for a relatively short duration with varying dropout rates between groups after postoperative 6 months and it was difficult to assess long-term disease progression or complications. Fourth, the study may be underpowered by a relatively small sample size. Finally, the results of the study may not be generalized to other ethnicities as the study population consisted of a single homogenous ethnicity (Korean), among whom normal tension glaucoma is known to be more prevalent. Nonetheless, the study suggests advantages of using MMC during AGV implantation with CS tube placement. We suggest further analysis on this topic with more patients, balanced groups, and detailed follow-up data.
In conclusion, during CS AGV implantation in eyes on maximum tolerated medical therapy for uncontrolled glaucoma, the intraoperative use of MMC reduced IOP in the 1st postoperative month compared to no use of MMC, but did not improve IOP control thereafter for 6 months after surgery.
Notes
Conflicts of Interest: Chan Yun Kim is the Editor-in-Chief of the Korean Journal of Ophthalmology since 2020. However, he was not involved in the peer reviewer selection, evaluation, or decision process of this article. No other potential conflicts of interest relevant to this article were reported.
Funding: This work was supported by the Basic Science Research Program (No. NRF-2019 R1A2C1091089) through the National Research Foundation of Korea (NRF). The funding organization had no role in the design or conducting of this research. None of the authors have any commercial or proprietary interests in any of the instruments or materials described in this study.
References
1. Barbosa-Breda J, Goncalves-Pinho M, Santos JV, et al. Trends in glaucoma surgical procedures in Portugal: a 16-year nationwide study 2000-2015. J Glaucoma 2018;27:682-6.


2. Lee CK, Ma KT, Hong YJ, Kim CY. Long-term clinical outcomes of Ahmed valve implantation in patients with refractory glaucoma. PLoS One 2017;12:e0187533.



3. Gedde SJ, Schiffman JC, Feuer WJ, et al. Treatment outcomes in the Tube Versus Trabeculectomy (TVT) study after five years of follow-up. Am J Ophthalmol 2012;153:789-803.



4. Gedde SJ, Herndon LW, Brandt JD, et al. Postoperative complications in the Tube Versus Trabeculectomy (TVT) study during five years of follow-up. Am J Ophthalmol 2012;153:804-14.



5. Topouzis F, Coleman AL, Choplin N, et al. Follow-up of the original cohort with the Ahmed glaucoma valve implant. Am J Ophthalmol 1999;128:198-204.

6. Kim JY, Lee JS, Lee T, et al. Corneal endothelial cell changes and surgical results after Ahmed glaucoma valve implantation: ciliary sulcus versus anterior chamber tube placement. Sci Rep 2021;11:12986.




7. Arikan G, Akbulut B, Utine CA, et al. Ahmed glaucoma valve implantation with the tube placement in the ciliary sulcus: short-term results. Int Ophthalmol 2022;42:969-80.



8. Bayer A, Onol M. Clinical outcomes of Ahmed glaucoma valve in anterior chamber versus ciliary sulcus. Eye (Lond) 2017;31:608-14.




9. Eslami Y, Mohammadi M, Fakhraie G, et al. Ahmed glaucoma valve implantation with tube insertion through the ciliary sulcus in pseudophakic/aphakic eyes. J Glaucoma 2014;23:115-8.


10. Godinho G, Barbosa-Breda J, Oliveira-Ferreira C, et al. Anterior chamber versus ciliary sulcus Ahmed glaucoma valve tube placement: longitudinal evaluation of corneal endothelial cell profiles. J Glaucoma 2021;30:170-4.


11. Costa VP, Azuara-Blanco A, Netland PA, et al. Efficacy and safety of adjunctive mitomycin C during Ahmed glaucoma valve implantation: a prospective randomized clinical trial. Ophthalmology 2004;111:1071-6.


12. Cui QN, Hsia YC, Lin SC, et al. Effect of mitomycin c and 5-flurouracil adjuvant therapy on the outcomes of Ahmed glaucoma valve implantation. Clin Exp Ophthalmol 2017;45:128-34.



13. Perez CI, Verdaguer S, Khaliliyeh D, et al. Subconjunctival injections of mitomycin C are associated with a lower incidence of hypertensive phase in eyes with Ahmed glaucoma valve. Ophthalmol Glaucoma 2021;4:322-9.


14. Jung KI, Park CK. Risk factors for the hypertensive phase after implantation of a glaucoma drainage device. Acta Ophthalmol 2016;94:e260-7.


15. Ederer F, Gaasterland DA, Dally LG, et al; The Advanced Glaucoma Intervention Study (AGIS): 13. Comparison of treatment outcomes within race: 10-year results. Ophthalmology 2004;111:651-64.


16. Jeong HJ, Park HL, Park CK. Effects of early postoperative intraocular pressure after Ahmed glaucoma valve implantation on long-term surgical outcomes. Korean J Ophthalmol 2018;32:391-9.




17. Won HJ, Sung KR. Hypertensive phase following silicone plate Ahmed glaucoma valve implantation. J Glaucoma 2016;25:e313-7.


18. Nouri-Mahdavi K, Caprioli J. Evaluation of the hypertensive phase after insertion of the Ahmed glaucoma valve. Am J Ophthalmol 2003;136:1001-8.


19. Abe RY, Tavares CM, Schimiti RB, et al. Ahmed glaucoma valve implantation for refractory glaucoma in a tertiary hospital in Brazil. J Ophthalmol 2015;2015:850785.




20. Yazdani S, Mahboobipour H, Pakravan M, et al. Adjunctive mitomycin C or amniotic membrane transplantation for Ahmed glaucoma valve implantation: a randomized clinical trial. J Glaucoma 2016;25:415-21.


21. Fargione RA, Tansuebchueasai N, Lee R, Tania Tai TY. Etiology and management of the hypertensive phase in glaucoma drainage-device surgery. Surv Ophthalmol 2019;64:217-24.


22. Alvarado JA, Hollander DA, Juster RP, Lee LC. Ahmed valve implantation with adjunctive mitomycin C and 5-fluorouracil: long-term outcomes. Am J Ophthalmol 2008;146:276-84.


23. Mietz H, Addicks K, Diestelhorst M, Krieglstein GK. Extraocular application of mitomycin C in a rabbit model: cytotoxic effects on the ciliary body and epithelium. Ophthalmic Surg 1994;25:240-4.


Fig.┬Ā1
Kaplan-Meier survival plots to compare surgical failure rates between mitomycin C (MMC) and no MMC groups. Surgical failure was defined as intraocular pressure exceeding 21 mmHg in two consecutive visits after postoperative 3 months, intraocular pressure Ōēż5 mmHg in two consecutive visits, or loss of light perception. A p-value of <0.05 was considered statistically significant according to log-rank test.
Table┬Ā1
Comparison of baseline characteristics
| Characteristic | No MMC group (n = 22) | MMC group (n = 32) | p-value* |
|---|---|---|---|
| Age (yr) | 65.2 ┬▒ 13.1 | 67.6 ┬▒ 14.1 | 0.532 |
| Male | 13 (59.1) | 18 (56.3) | 0.999 |
| Right eye | 11 (50.0) | 16 (50.0) | 0.999 |
| Central corneal thickness (╬╝m) | 537.4 ┬▒ 39.3 | 539.6 ┬▒ 25.0 | 0.828 |
| Axial length (mm) | 25.0 ┬▒ 2.9 | 25.0 ┬▒ 2.7 | 0.992 |
| Familial history | 2 (9.1) | 4 (12.5) | 0.999 |
| Phakic eye | 3 (16.7) | 4 (12.5) | 0.999 |
| Type of glaucoma | 0.789 | ||
| ŌĆāPrimary open angle glaucoma | 8 (36.4) | 13 (40.6) | |
| ŌĆāPrimary angle closure glaucoma | 2 (9.1) | 2 (6.3) | |
| ŌĆāPseudoexfoliation glaucoma | 5 (22.7) | 10 (31.3) | |
| ŌĆāNeovascular glaucoma | 2 (9.1) | 3 (9.4) | |
| ŌĆāUveitic | 2 (9.1) | 3 (9.4) | |
| ŌĆāPigmentary | 3 (16.7) | 1 (3.1) | |
| Systemic disease | |||
| ŌĆāHypertension | 8 (36.4) | 20 (62.5) | 0.107 |
| ŌĆāDiabetes mellitus | 8 (36.4) | 13 (40.6) | 0.975 |
| ŌĆāCerebrovascular disease | 0 (0) | 2 (6.3) | 0.508 |
| Preoperative RNFL thickness (╬╝m) | 71.8 ┬▒ 23.0 | 72.1 ┬▒ 23.8 | 0.968 |
| Preoperative MD (dB) | ŌłÆ17.0 ┬▒ 8.6 | ŌłÆ15.9 ┬▒ 9.6 | 0.681 |
| Preoperative VFI (%) | 52.8 ┬▒ 30.5 | 55.6 ┬▒ 32.4 | 0.763 |
| Follow-up duration (yr) | 2.2 ┬▒ 1.1 | 1.0 ┬▒ 0.1 | <0.001 |
Table┬Ā2
Mean IOP and percent reduction following ciliary sulcus Ahmed glaucoma valve tube placement depending on the use of intraoperative MMC at all time intervals
| Follow-up | Average IOP (mmHg) | IOP reduction (%) | ||||
|---|---|---|---|---|---|---|
|
|
|
|||||
| No MMC group (n = 22) | MMC group (n = 32) | p-value* | No MMC group (n = 22) | MMC group (n = 32) | p-value* | |
| Preoperative | 26.8 ┬▒ 8.0 | 27.2 ┬▒ 8.0 | 0.857 | - | - | - |
| 1 wk | 10.8 ┬▒ 4.8 | 11.6 ┬▒ 7.1 | 0.643 | 56.0 ┬▒ 20.8 | 54.7 ┬▒ 28.3 | 0.863 |
| 1 mon | 20.5 ┬▒ 8.6 | 15.8 ┬▒ 6.4 | 0.027 | 16.6 ┬▒ 45.8 | 38.0 ┬▒ 28.8 | 0.042 |
| 3 mon | 14.6 ┬▒ 3.8 | 14.4 ┬▒ 3.3 | 0.870 | 39.8 ┬▒ 26.3 | 43.0 ┬▒ 19.6 | 0.956 |
| 6 mon | 14.4 ┬▒ 4.8 | 14.7 ┬▒ 2.7 | 0.805 | 40.5 ┬▒ 29.1 | 42.1 ┬▒ 19.9 | 0.821 |
Table┬Ā3
Comparisons of the average number of antiglaucoma medications during follow-up between MMC and no MMC groups
| Follow-up | No MMC group (n = 22) | MMC group (n = 32) | p-value* |
|---|---|---|---|
| Preoperative | 2.7 ┬▒ 0.5 | 2.3 ┬▒ 1.0 | 0.062 |
| 1 wk | 0 | 0 | - |
| 1 mon | 1.4 ┬▒ 0.9 | 0.8 ┬▒ 1.0 | 0.047 |
| 3 mon | 1.6 ┬▒ 0.9 | 1.4 ┬▒ 1.1 | 0.354 |
| 6 mon | 1.6 ┬▒ 0.9 | 1.5 ┬▒ 1.1 | 0.786 |
Table┬Ā4
Postoperative complications following ciliary sulcus Ahmed glaucoma valve implantation depending on the use of MMC during surgery
| Complication | No MMC group (n = 22) | MMC group (n = 32) | p-value* |
|---|---|---|---|
| Hyphema | 5 (22.7) | 11 (34.4) | 0.537ŌĆĀ |
| Conjunctival leakage | 0 (0) | 1 (3.1) | 0.999ŌĆĪ |
| Flat anterior chamber | 1 (4.5) | 1 (3.1) | 0.999ŌĆĪ |



 PDF Links
PDF Links PubReader
PubReader ePub Link
ePub Link Full text via DOI
Full text via DOI Full text via PMC
Full text via PMC Download Citation
Download Citation Print
Print




