Dear Editor,
Management of endothelial dysfunction with coexisting cataract have been reported with several surgical methods in abroad. According to these reports, 3-step procedure with concurrent cataract extraction, intraocular lens implantation and Descemet membrane endothelial keratoplasty (DMEK), in other words, triple DMEK, do not represent higher risk of any complications than DMEK alone [1-4]. In patients 50 years or older, combined cataract surgery is recommended because of need of cataract surgery after DMEK [5]. We already know that there are several cases of triple DMEK in Korea. Nevertheless, we cannot found reports about this triple DMEK in Korea, so we would like to introduce a successful case in our hospital.
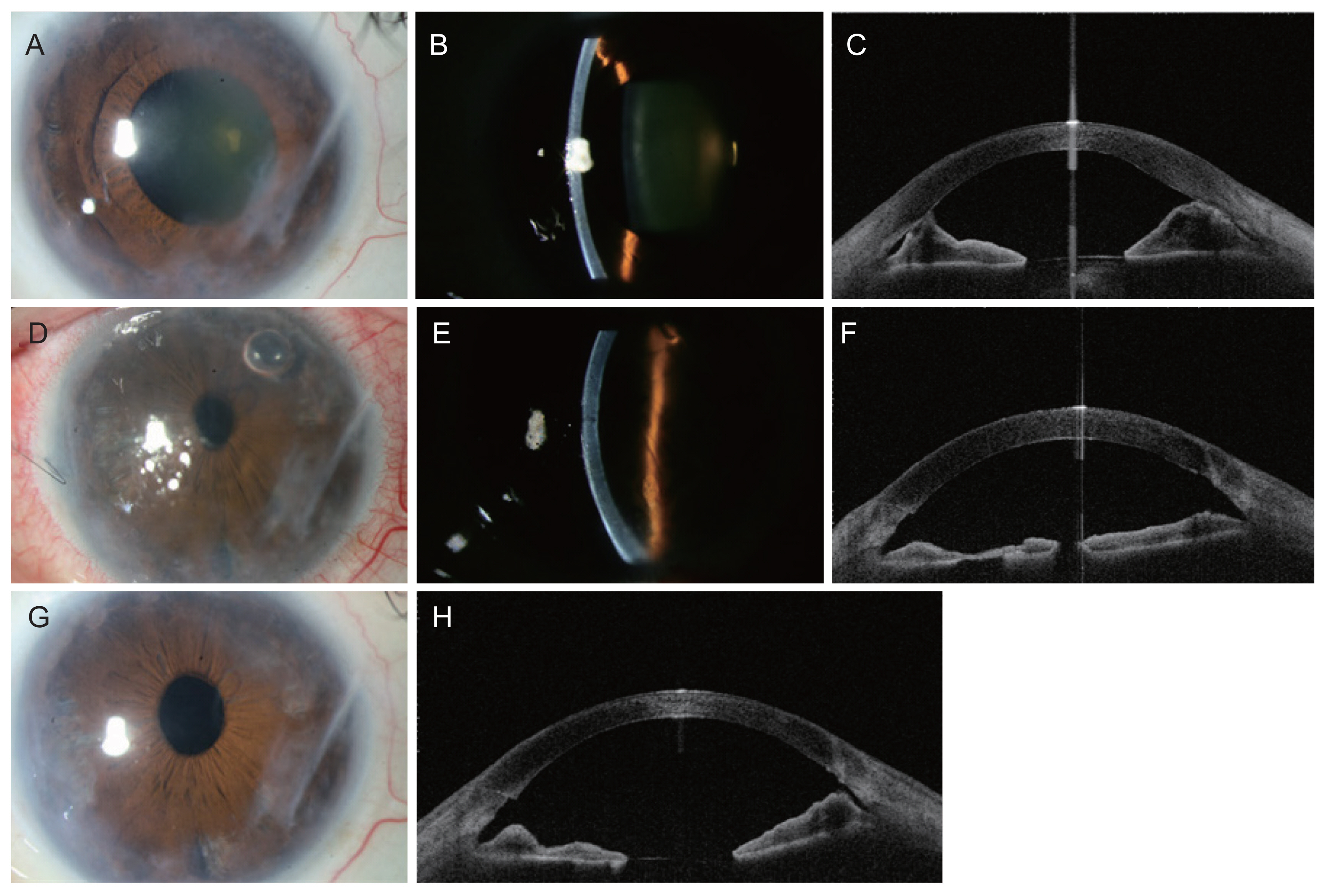
We report a case of post-traumatic corneal endothelial dysfunction successfully treated with triple DMEK surgery. A 51-year-old man was referred for impaired vision for 18 months. He had trauma history at 35 years ago that his right eye was hit by a baseball and the cornea was lacerated with glasses, and it was primary repaired immediately at local clinic. He had been examined at other hospital for traumatic cataract, endothelial dysfunction and peripheral anterior synechiae (PAS) since 2019, and referred to our clinic. At the initial visit, his best-corrected visual acuity (BCVA) was 20 / 32 in his right eye. On specular microscopy, cell density of his right eye was 683 per mm3 and coefficient of variation was 34. Slit lamp examination and CASIA (Tomey Corp., Nagoya, Japan) swept-source anterior segment optical coherence tomography showed 360┬░ PAS, corneal opacity, corneal edema, and cataract in the right eye (Fig. 1A-1C).
We planned triple DMEK on his right eye. He requested cataract surgery on his left eye simultaneously, because of the expected discomfort with postoperative anisometropia. As a result, he underwent simultaneous DMEK on his right eye and cataract surgery on his both eyes. Donor graft was prepared as precut, 8.00 mm sized. A side puncture was made and ophthalmic viscoelastic device (OVD) was injected in anterior chamber. A 2.8-mm-sized corneal incision was made on temporal side and anterior synechiolysis was attempted with the size of over 8.0 mm, especially at nasal half. We made smaller capsulorrhexis than usual cataract surgery. Routine cataract surgery was performed with careful polishing, and hydrophobic acrylic 1-piece intraocular lens. After additional anterior synechiolysis, Descemet membrane stripping was done within OVD-filled anterior chamber and dilated pupil. Remaining OVD was removed precisely. Manual meiosis with peripheral iridotomy was made, and the rest steps of DMEK was performed as usual.
On 1 day after surgery, BCVA was 20 / 500 and intraocular pressure (IOP) was 13.8 mmHg in his right eye. Anterior synechiae was almost released and Descemet membrane was well attached (Fig. 1D-1F). One month after surgery, BCVA was 20 / 25 and IOP was 15.2 mmHg in his right eye. On specular microscopy of his right eye, cell density was 2,203 per mm3 and coefficient of variation was 28. Corneal opacity was significantly reduced (Fig. 1G). Released anterior synechiae on anterior segment optical coherence tomography was maintained (Fig. 1H). Two months after surgery, BCVA was 20 / 22 and IOP was 14.9 mmHg in his right eye.
In surgical planning of the cases like this, we would like to recommend some critical matters. Firstly, capsulorrhexis should be smaller than the usual cataract cases. To prevent intraocular lens touch of DMEK graft, we think capsulorrhexis might be done 4.5 mm or smaller during triple DMEK operation. Second is minimal use of OVD and complete removal of OVD before DMEK surgery. If OVD is remaining in anterior chamber after cataract surgery, the unfolded DMEK graft may not attach well the stromal bed. Lastly, when PAS was found before the DMEK surgery, DMEK graft size should be carefully determined considering that if the PAS is dense, it can be removed incompletely. So, the size should be smaller than the usual DMEK graft. In conclusion, triple DMEK procedure represents rapid visual rehabilitation and stable postoperative condition. We also can provide cost-effectiveness for shorter admission duration and additional efforts required for operation, such as nurses or anesthesiologist. If skillful surgeons carefully consider for critical matters above, triple DMEK seems to make lesser endothelial damage and show no significant effect on refraction due to the nature of DMEK.



 PDF Links
PDF Links PubReader
PubReader ePub Link
ePub Link Full text via DOI
Full text via DOI Full text via PMC
Full text via PMC Download Citation
Download Citation Print
Print






