Dear Editor,
Malignant peripheral nerve sheath tumor (MPNST) is an uncommon soft tissue sarcoma that arises from peripheral nerves. MPNST of the orbit is very rare and only accounts for 0% to 0.2% of all orbital tumors. About 70% of MPNSTs are associated with neurofibromatosis type 1 (NF-1) and benign neurofibromas rarely undergo malignant transformation. As far as the authors know there has been only one report of an orbital MPNST arising from a benign neurofibroma. Here, we report a patient with MPNST arising from a benign neurofibroma who showed long survival with surgical excision and radiation.
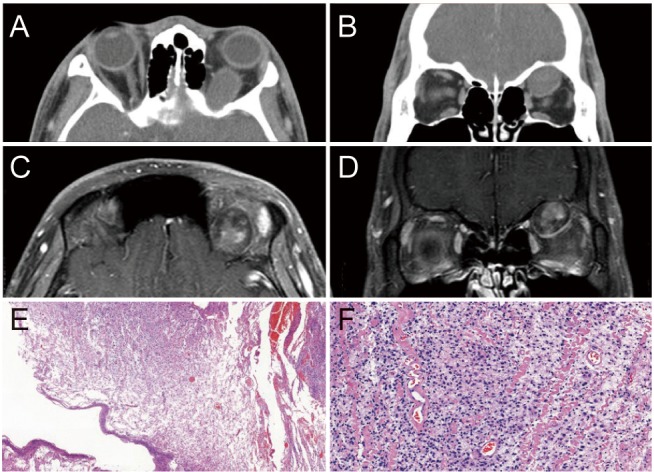
A 19-year-old male visited our clinic for a left eye proptosis lasting 4 months. On examination, visual acuity in his left eye was 20 / 20 and exophthalmometric values were 16 mm on the right eye and 20.5 mm on the left eye. The exophthalmic left eye showed limited upward gaze. Computed tomography scan revealed an extraconal 22 × 18 × 42-mm-sized mass between the superior rectus muscle and the superior orbital wall with peripheral wall enhancement and central mottled enhancement (Fig. 1A, 1B). Magnetic resonance imaging with dynamic contrast enhancement showed a well-defined and spindle-shaped mass with low signal intensity on T1-weighted images and high signal intensity on T2-weighted images. After contrast enhancement, mottled enhancement was observed in the central portion of the tumor that gradually increased over time (Fig. 1C, 1D).
Surgical excision was performed through superior orbitotomy. After opening the superior periorbita, the mass was exposed. The mass was carefully dissected and removed. Pathologic examination revealed small round cells with increased cellularity and a fibrillary background. Mitotic count was two per 10 high power fields and the resection margin was associated with a neurofibroma (Fig. 1E, 1F). Immunohistochemistry revealed cells positive for vimentin, S-100, neuron specific enolase, suggestive of a neural origin. Immunonegativity of desmin and smooth muscle actin helped rule out the possibility of tumors of muscular origin. Based on these findings, the patient was diagnosed with low grade MPNST in the background of neurofibroma. The patient received adjuvant fractionated stereotactic radiotherapy to the left orbit. He has been disease-free without recurrence until the last follow-up (7 years postoperatively).
MPNSTs are known to originate from cells constituting the nerve sheath including perineural fibroblasts or Schwann cells. NF-1 and irradiation history are known risk factors for MPNST. The prevalence of MPNST in patients with NF-1 is 4% and 0.001% in the general population [1]. MPNSTs generally arise de novo but may also arise as a consequence of malignant transformation of a neurofibroma. There is only one reported case of malignant transformation of a neurofibroma in the orbit of a patient without NF-1 and this is a second case [2].
On computed tomography, MPNSTs often appear as well-defined, rounded, homogenously enhancing masses and these tumors may be found to erode adjacent bony structures. These findings were also observed in our case. On magnetic resonance imaging, MPNSTs have an isointense homogenous signal intensity on T1-weighted images, and necrotic lesions show high signal intensity on T2-weighted images [3]. In our case, the tumor showed low signal intensity on T1-weighted images and high signal intensity on T2-weighted images.
The definitive diagnosis of MPNST is obtained by biopsy. MPNSTs are highly cellular and composed of spindle-shaped cells which have active cell division and atypical nuclei [4]. Immunohistochemical staining can be helpful for diagnosis when it shows a positive response for neural antigens including vimentin, S-100 protein, neuron-specific enolase and neurofilaments, and a negative response for antibodies associated with differentiation of epithelial cells, neuroendocrine cells, or muscle cells [5].
The main treatment is surgical excision and wide excision of the primary site should be done. If there is intracranial invasion, orbital exenteration with craniotomy is suggested. Radiation therapy is recommended after surgery, especially when complete resection is difficult or when the resection margin is uncertain [2].
We report a case of MPNST arising from a neurofibroma. Our case showed long-term survival after surgical excision and postoperative radiation therapy, and this is thought to be due to complete tumor excision. Although the incidence of MPNST is very rare, it should be included in the differential diagnosis of rapid-growing orbital masses.



 PDF Links
PDF Links PubReader
PubReader Full text via DOI
Full text via DOI Full text via PMC
Full text via PMC Download Citation
Download Citation Print
Print






