Central serous chorioretinopathy (CSC) is a disorder characterized by serous detachment of the neurosensory retina from the retinal pigment epithelium (RPE) and is often associated with diffuse RPE atrophy. CSC is approximately six times more prevalent in men than in women [
1,
2]. Although the exact pathophysiology of CSC is yet to be determined, CSC is known to be related to personality (i.e., type A), anxiety, and stress [
3,
4,
5,
6,
7,
8], and stress-induced hypercortisolism may contribute to the development of CSC [
9].
CSC is classically divided into two phases (active and inactive) and two subtypes (acute and chronic). Although many studies have investigated the association of active CSC with psychological factors [
5,
7,
10,
11], the association of inactive CSC with psychological factors has received much less consideration. Furthermore, the subtype of CSC was not considered in the previous studies on the association of CSC with psychological factors, despite the differences in pathological and clinical characteristics of acute and chronic CSC. Acute CSC is characterized by serous retinal detachment accompanied by limited focal or multifocal RPE changes and often resolves within 3 to 4 months with a favorable visual outcome. In contrast, the chronic form of CSC, also known as diffuse retinal pigment epitheliopathy, is characterized by widespread RPE atrophy and has a poor visual outcome [
1]. Choroidal vascular hyperpermeability is one of the key pathologies in CSC and has been associated with the severity and/or activity of CSC [
12,
13]. However, the associations between vascular hyperpermeability in CSC and psychosocial factors have not been thoroughly studied.
In this study, we investigated the psychological factors associated with CSC according to phase and subtype. In addition, we analyzed the correlations between psychological factors and the extent of choroidal hyperpermeability as measured by indocyanine green angiography (ICGA).
Materials and Methods
Participants
Participants were consecutively enrolled from those with CSC visiting the ophthalmology outpatient clinic of Seoul National University Bundang Hospital between October 26, 2012 and February 28, 2015. Patients were excluded if any of the following were present: another ophthalmic disorder that might affect vision and/or foveal structure (e.g., age-related macular degeneration, diabetic retinopathy, retinal vascular obstruction, or uveitis); a history of intraocular surgery other than uncomplicated cataract surgery; or inability to read and respond to the questionnaire. Age- and sex-matched healthy volunteers without a history of ocular disease were enrolled from the Medical Check-up Center of Seoul National University Bundang Hospital during the same period. All subjects provided informed consent. This study was approved by the institutional review board of Seoul National University Bundang Hospital, Seongnam, South Korea) (B-1208/166-009). All study conduct adhered to the tenets of the Declaration of Helsinki, and written informed consent was obtained from all study participants.
Ophthalmologic evaluation
Patients underwent examination by slit lamp, fundoscopy, optical coherence tomography (OCT; Spectralis OCT, Heidelberg Engineering, Heidelberg, Germany), fluorescein angiography, and/or ICGA (Heidelberg Retina Angiography, Heidelberg Engineering). One skilled observer (YKK) manually measured the size of the hyperpermeable choroidal lesion on ICGA using the built-in caliper tool. The size of the hyperpermeable choroidal lesion was defined as the diameter of the smallest circle covering the main hyperpermeable choroidal lesion, as identified on mid-to late-phase ICGA and that resulted in accumulation of subretinal fluid. We selected mid-to late-phase ICGA images that revealed prominent vascular leakage or punctate hyperfluorescence spots. Using the built-in caliper tool, we drew the smallest circle that covered all hyperpermeable lesions for each image. If the patient had two distinct hyperpermeable choroidal lesions, the two were measured separately, and the lesion sizes were summed (
Fig. 1A, 1B).
Psychosocial evaluation
We evaluated state and trait anxiety using the State-Trait Anxiety Inventory [
14,
15]. The State-Trait Anxiety Inventory has 20 items for assessing trait anxiety and 20 items for assessing state anxiety. Each item is rated on a 4-point scale; higher scores indicate greater anxiety levels. We evaluated depressive symptoms using the Beck Depression Inventory, which consists of 21 items [
16]. Higher scores indicate that the subject is more depressed. We evaluated major life stressors that patients had experienced using the Social Readjustment Rating Scale [
17]. This questionnaire consists of 43 stressful life events that patients might have experienced within the past 12 months. Higher scores indicate that the subject is experiencing more cumulative stress due to life events. We evaluated stress coping strategies using the Coping Inventory for Stressful Situations [
18]. This instrument consists of 48 items that distinguish between three basic coping strategies with 16 items per scale: task-oriented (T scale), emotion-oriented (E scale), and avoidance (A scale). We evaluated perceived social support using the Medical Outcomes Study Social Support Survey [
19]. All instruments were self-administered questionnaires.
Diagnosis and classification of CSC
We diagnosed CSC based on findings on fundoscopy, fluorescein angiography, ICGA, and OCT. Patients who had subretinal fluid with active leakage on fluorescein angiography and choroidal vascular hyperpermeability as seen on ICGA were classified as having active CSC. Those with a history of CSC confirmed by medical records, but no current subretinal fluid on OCT or active leakage on fluorescein angiography were classified as having inactive CSC. We also classified active CSC into subtypes according to the presence or absence of widespread RPE atrophy. Acute CSC was defined as CSC with focal RPE atrophy (less than 1-disc area). Subretinal fluid of this subtype usually resolved spontaneously within 3 months. We also included patients who underwent photodynamic therapy due to persistent subretinal fluid in this category, unless they are accompanied by widespread RPE atrophy. Chronic CSC was defined as a chronic disease course of recovery and relapse accompanied by widespread RPE atrophy (larger than 1-disc area).
Statistical analyses
We compared the demographic and psychometric characteristics between the CSC and control groups using the Mann-Whitney U-test. We examined the correlation between choroidal hyperpermeable lesion size and psychosocial characteristics using Pearson's correlation test. The statistical analyses were performed using Stata ver. 13.0 (Stata Corp, College Station, TX, USA). Statistical significance was defined as p < 0.05, and borderline significance was defined as p Ōēź 0.05 and p < 0.08.
Results
In this study, we recruited 37 CSC patients and 37 age- and sex-matched controls. Of the 37 CSC patients, 19 were in the active phase and 18 were in the inactive phase at the time of enrollment. Of the 19 active CSC patients, 10 were classified as acute CSC without any history of previous CSC events, and 9 were classified as chronic CSC with a relapsing course of disease accompanied by large RPE atrophy. All inactive patients had previous history of more than two CSC recurrences that subsided spontaneously or following photodynamic therapy. At the time of enrollment, no activity (no subretinal fluid) was observed in the eyes of the inactive patients.
As summarized in
Table 1, the CSC group showed higher state anxiety (45.9 ┬▒ 12.9 vs. 40.3 ┬▒ 9.6,
p = 0.036) scores, stress (532.2 ┬▒ 599.1 vs. 263.3 ┬▒ 280.5,
p = 0.016) scores, and borderline high depression (11.8 ┬▒ 7.6 vs. 8.1 ┬▒ 8.8,
p = 0.059) scores compared to the control group. Their active stress coping (99.2 ┬▒ 18.4 vs. 106.7 ┬▒ 18.0,
p = 0.080) and perceived emotional support (54.8 ┬▒ 22.0 vs. 63.3 ┬▒ 18.1,
p = 0.072) scores were borderline lower than those of the control group. Analyzing patients with active CSC and inactive CSC separately, we discovered that the active CSC group showed higher stress (453.4 ┬▒ 531.5 vs. 192.0 ┬▒ 210.8,
p = 0.030) and depression (11.5 ┬▒ 6.8 vs. 8.6 ┬▒ 11.1,
p = 0.037) scores and lower emotional support (47.9 ┬▒ 22.2 vs. 65.1 ┬▒ 20.7,
p = 0.014) and informational support (51.3 ┬▒ 22.0 vs. 66.1 ┬▒ 18.0,
p = 0.022) scores than their age- and sex-matched controls. However, such differences were not found between the inactive CSC group and the control group (
Table 1).
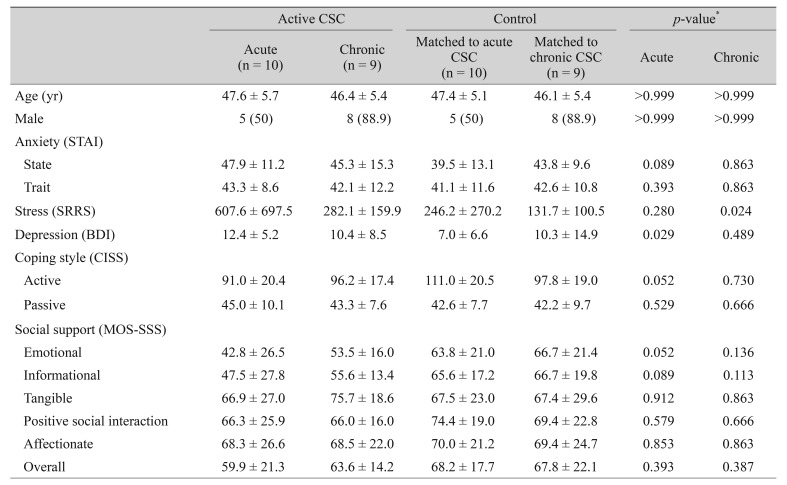
When we further divided the active CSC group into acute and chronic subtypes, the acute active CSC patients showed a higher depression score (12.4 ┬▒ 5.2 vs. 7.0 ┬▒ 6.6,
p = 0.029), while the chronic active CSC patients showed a higher stress score (282.1 ┬▒ 159.9 vs. 131.7 ┬▒ 100.5,
p = 0.024) than their age- and sex-matched control groups. The acute active CSC group also showed lower active stress coping (91.0 ┬▒ 20.4 vs. 111.0 ┬▒ 20.5,
p = 0.052) and perceived emotional support (42.8 ┬▒ 26.5 vs. 63.8 ┬▒ 21.0,
p = 0.052) scores with borderline significance (
Table 2).
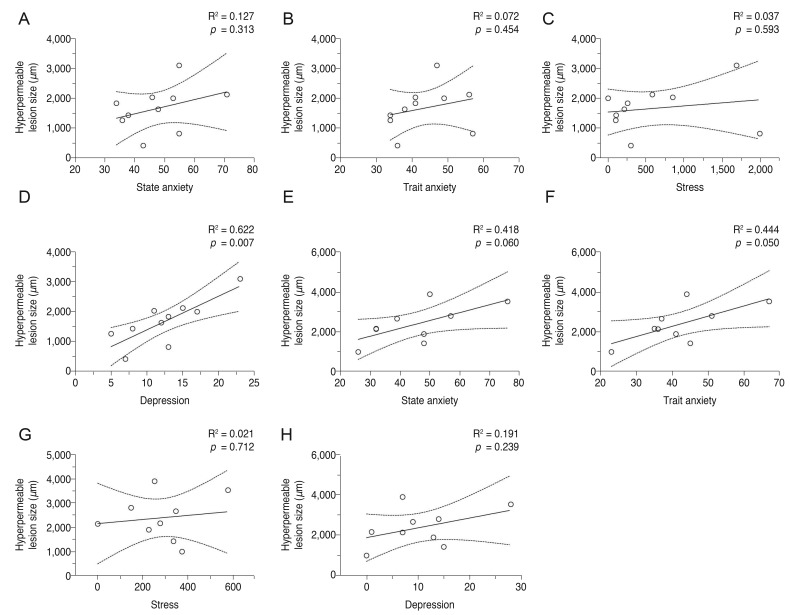
Size of the hyperpermeable choroidal lesion was correlated with depression score (r = 0.789,
p = 0.007) in the acute CSC group. Lesion size was correlated with state anxiety score (r = 0.647,
p = 0.060) and trait anxiety score (r = 0.666,
p = 0.050) in the chronic CSC group with borderline significance (
Fig. 2A-2H).
Discussion
In this study, we found that psychosocial factors such as anxiety, depression, or stress were associated with CSC in the active phase but not in the inactive phase. We also found that the psychosocial factors associated with active CSC were different between acute and chronic subtypes. Acute CSC was associated with depression, inadequate stress coping, and less social support. On the other hand, chronic CSC was associated with stress.
In all previous studies except one [
20], patients with CSC were found to be more prone to emotional distress or illness-related work stress [
5,
7,
10,
11], possibly because of their inadequate coping strategies [
10] or low perceived social support [
5,
21]. However, most of these studies were conducted on patients with active CSC; the subtype of CSC was not considered. The various psychosocial factors that were associated with CSC in previous studies can be either traits or states of people with CSC. If the association of CSC with psychosocial factors is different according to phase, i.e., active or inactive, one could ascertain whether the psychosocial factors are trait or state markers of the disease.
This study suggests that anxiety, depression, and stress are associated with CSC in the active phase but not in the inactive phase, thus supporting the proposition that these psychological factors are state markers of CSC. After analyzing acute and chronic CSC separately, we determined that acute CSC was associated with depression, while chronic CSC was associated with stress. Patients with acute CSC showed less active-stress coping, felt lack of emotional support, and were more depressive than the normal controls. Although this study was cross-sectional and could not show a causal relationship between depression and acute CSC, enhancement of coping skills and/or enrichment of emotional support may be helpful in reducing the risk or severity of acute CSC.
On the other hand, chronic CSC was associated with stress. All other psychosocial factors we evaluated were comparable with those of the control group. Although the active coping and perceived emotional support in the chronic CSC group were slightly lower than those in the normal control group, the differences did not reach statistical significance. Chronic CSC develops in older patients who have a greater incidence of bilateral involvement and are more likely to develop secondary choroidal neovascularization [
1]. There have been a few studies that directly compared the psychosocial characteristics between acute and chronic CSC. Lahousen et al. [
22] reported that patients with acute CSC had more psychosomatic complaints and negative stress coping but a comparable number of critical life events before diagnosis compared with chronic CSC. Tittl et al. [
2] reported that patients with chronic CSC were more likely to use anxiolytics or antidepressants than normal controls, but those with acute CSC were not.
Interestingly, in acute CSC patients, the severity of depression showed good linear correlation with the size of the choroidal pathology. Inappropriate activation of the mineralocorticoid receptor (MR) in choroidal endothelial cells has been recently suggested as a molecular mechanism for choroidal vasodilation in CSC [
23,
24], and MR antagonists have shown promising results in the treatment of non-resolving CSC cases [
25,
26,
27]. It is also known that the MR plays an important role in the hypothalamic-pituitary-adrenal axis and is a principal mediator in stress, which is also a predisposing factor in the development of depression [
28,
29]. There might be an association between depression and acute CSC via inappropriate MR activation, and further study is needed to prove this hypothesis. However, in chronic CSC patients, both state and trait anxiety levels showed marginal linear correlation with the size of the hyperpermeable choroidal lesion. The stress level, which was significantly higher in the chronic CSC group compared to age- and, sex-matched controls, did not show significant correlation with the size of the hyperpermeable choroidal lesion.
In this study, we measured the frequency of stressful life events, and the degree of stress perceived by individuals might have varied according to their mechanisms for coping and/or their degree of social support. Indeed, a previous report showed a weak correlation between the number of critical life events and a patient's distress as measured by the Symptom Checklist-90-R [
11]. In certain circumstances, such as a relapsing eye disease accompanied by stressful life events, anxiety might predispose patients to the chronic state of the disease. Anxiety is thought to be an essential feature of CSC [
6,
8,
30], and further research on the role of anxiety in the development or progression of CSC might be needed.
In this study, we only included patients with documented subretinal fluid on previous OCT images, confirming the diagnosis of CSC in currently inactive patients. However, some of the patients might harbor the characteristics of pachychoroid pigment epitheliopathy or pachychoroid neovasculopathy, which share clinical and pathophysiological features with CSC [
31,
32]. Once the diagnostic criteria for these diseases are established, a comparative study might be needed to determine any differences in the psychosocial state of these patients and CSC patients.
This study has several limitations. First, this study was cross-sectional and therefore could not determine a causal relationship between CSC and psychosocial factors. Second, the sample size was small, but the age- and sex-matched controls enrolled in this study might have improved the statistical power. Third, we did not measure the numbers of critical life events. However, we evaluated the stressful life events within 12 months of CSC onset, which may be more inf luential on CSC than lifetime events. Fourth, all inactive patients in this study experienced several recurrences during the follow-up period. Further studies that include patients who recovered from acute CSC without recurrence might be needed to better elucidate the psychological status of inactive CSC patients. Fifth, we could not analyze the psychosocial features of CSC patients according to recurrence history, such as the number of relapses or the duration of the disease-free period, due to the small number of cases. Finally, we did not examine the use of psychotropic medications.
In conclusion, psychosocial factors were associated with CSC in the active phase. However, the psychosocial factors that were associated with acute CSC were different from those associated with chronic CSC. In acute active CSC, severity of depression was correlated with the size of the choroidal pathology. Further studies with a prospective design are warranted to determine if psychosocial factors can trigger CSC and the mechanism of provocation.
Acknowledgements
This work was supported by grants from the National Research Foundation of Korea (NRF) funded by the Korean government (Ministry of Science, ICT and Future Planning) (2010-0028631 and 2016R1D1A1B03934724) and a grant from Seoul National University Bundang Hospital (11-2012-017). The funding organization had no role in the design or conduct of this research.
Notes
Conflict of Interest: No potential conflict of interest relevant to this article was reported.
REFERENCES
1. Spaide RF, Campeas L, Haas A, et al. Central serous chorioretinopathy in younger and older adults.
Ophthalmology 1996;103:2070-2079.


2. Tittl MK, Spaide RF, Wong D, et al. Systemic findings associated with central serous chorioretinopathy.
Am J Ophthalmol 1999;128:63-68.


3. Yannuzzi LA. Type-A behavior and central serous chorioretinopathy.
Retina 1987;7:111-131.


4. Tsai DC, Chen SJ, Huang CC, et al. Epidemiology of idiopathic central serous chorioretinopathy in Taiwan, 2001-2006: a population-based study.
PLoS One 2013;8:e66858.



5. Conrad R, Geiser F, Kleiman A, et al. Temperament and character personality profile and illness-related stress in central serous chorioretinopathy.
ScientificWorldJournal 2014;2014:631687.



6. Piskunowicz M, Jaracz M, Lesiewska H, et al. Temperament profile in patients with central serous chorioretinopathy: a case-control study.
Eur J Ophthalmol 2014;24:392-395.


7. Sahin A, Bez Y, Kaya MC, et al. Psychological distress and poor quality of life in patients with central serous chorioretinopathy.
Semin Ophthalmol 2014;29:73-76.


8. Bazzazi N, Ahmadpanah M, Akbarzadeh S, et al. In patients suffering from idiopathic central serous chorioretinopathy, anxiety scores are higher than in healthy controls, but do not vary according to sex or repeated central serous chorioretinopathy.
Neuropsychiatr Dis Treat 2015;11:1131-1136.


9. Caccavale A, Romanazzi F, Imparato M, et al. Central serous chorioretinopathy: a pathogenetic model.
Clin Ophthalmol 2011;5:239-243.



10. Conrad R, Bodeewes I, Schilling G, et al. Central serous chorioretinopathy and psychological stress.
Ophthalmologe 2000;97:527-531.


11. Conrad R, Weber NF, Lehnert M, et al. Alexithymia and emotional distress in patients with central serous chorioretinopathy.
Psychosomatics 2007;48:489-495.


12. Piccolino FC, Borgia L. Central serous chorioretinopathy and indocyanine green angiography.
Retina 1994;14:231-242.


13. Spaide RF, Hall L, Haas A, et al. Indocyanine green videoangiography of older patients with central serous chorioretinopathy.
Retina 1996;16:203-213.


14. Spielberger CD, Gorsuch RL, Lushene R, et al. Manual for the State-Trait Anxiety Inventory. Palo Alto: Consulting Psychologists Press; 1983.
15. Hahn DW, Lee CH, Chon KK. Korean adaptation of Spielberger's STAI (K-STAI). Korean J Health Psychol 1996;1:1-14.
16. Beck AT, Ward CH, Mendelson M, et al. An inventory for measuring depression.
Arch Gen Psychiatry 1961;4:561-571.


17. Holmes TH, Rahe RH. The social readjustment rating scale.
J Psychosom Res 1967;11:213-218.


18. Endler NS, Parker JD. Multidimensional assessment of coping: a critical evaluation.
J Pers Soc Psychol 1990;58:844-854.


19. Sherbourne CD, Stewart AL. The MOS social support survey.
Soc Sci Med 1991;32:705-714.


20. Spahn C, Wiek J, Burger T, Hansen L. Psychosomatic aspects in patients with central serous chorioretinopathy.
Br J Ophthalmol 2003;87:704-708.



21. Franke GH, Esser J, Stacker KH, et al. ŌĆ£Filtered normalityŌĆØ: psychological causes and sequelae of specific retinal diseases.
Psychother Psychosom Med Psychol 1996;46:159-168.

22. Lahousen T, Painold A, Luxenberger W, et al. Psychological factors associated with acute and chronic central serous chorioretinopathy.
Nord J Psychiatry 2016;70:24-30.


23. Zhao M, Celerier I, Bousquet E, et al. Mineralocorticoid receptor is involved in rat and human ocular chorioretinopathy.
J Clin Invest 2012;122:2672-2679.



24. Daruich A, Matet A, Dirani A, et al. Central serous chorioretinopathy: recent findings and new physiopathology hypothesis.
Prog Retin Eye Res 2015;48:82-118.


25. Bousquet E, Beydoun T, Rothschild PR, et al. Spironolactone for nonresolving central serous chorioretinopathy: a randomized controlled crossover study.
Retina 2015;35:2505-2515.



26. Daruich A, Matet A, Dirani A, et al. Oral mineralocorticoid-receptor antagonists: real-life experience in clinical subtypes of nonresolving central serous chorioretinopathy with chronic epitheliopathy.
Transl Vis Sci Technol 2016;5:2.

27. Ghadiali Q, Jung JJ, Yu S, et al. Central serous chorioretinopathy treated with mineralocorticoid antagonists: a one-year pilot study.
Retina 2016;36:611-618.


28. Young EA, Lopez JF, Murphy-Weinberg V, Watson SJ, Akil H. Mineralocorticoid receptor function in major depression.
Arch Gen Psychiatry 2003;60:24-28.


29. Chen J, Wang ZZ, Zhang S, Zuo W, Chen NH. Does mineralocorticoid receptor play a vital role in the development of depressive disorder?
Life Sci 2016;152:76-81.


30. Tsai DC, Chen SJ, Huang CC, et al. Risk of central serous chorioretinopathy in adults prescribed oral corticosteroids: a population-based study in Taiwan.
Retina 2014;34:1867-1874.


31. Warrow DJ, Hoang QV, Freund KB. Pachychoroid pigment epitheliopathy.
Retina 2013;33:1659-1672.


32. Pang CE, Freund KB. Pachychoroid neovasculopathy.
Retina 2015;35:1-9.


Fig.┬Ā1
Measurement of hyperpermeable choroidal lesion size. We measured the diameter of the smallest circle (dotted circles) that covered the main hyperpermeable choroidal lesions identified on mid-to late-phase indocyanine green angiography. (A) The white dotted circle covers the central main lesion. (B) The dotted circle covers all separated hyperpermeable lesions.

Fig.┬Ā2
Correlations between hyperpermeable choroidal lesion size and psychometric parameters in acute (A, state anxiety; B, trait anxiety; C, stress; D, depression) and chronic (E, state anxiety; F, trait anxiety; G, stress; H, depression) central serous chorioretinopathy (CSC) patients. (D) Depression scores showed significant correlation with the size of the hyperpermeable choroidal lesion in acute CSC. (E,F) State anxiety scores and trait anxiety scores showed borderline significant correlation with the size of the hyperpermeable choroidal lesion in chronic CSC.
Table┬Ā1
Demographics and psychometric parameters in patients with CSC and controls matched for age and sex

Table┬Ā2
Demographics and psychometric parameters in patients with active CSC and controls matched for age and sex










 PDF Links
PDF Links PubReader
PubReader Full text via DOI
Full text via DOI Full text via PMC
Full text via PMC Download Citation
Download Citation Print
Print



