 |
 |
| Korean J Ophthalmol > Volume 32(3); 2018 > Article |
Abstract
Purpose
To evaluate the agreement in axial length (AL), keratometry, and anterior chamber depth measurements between AL-Scan and IOLMaster biometers and to compare the efficacy of the AL-Scan on intraocular lens (IOL) power calculations and refractive outcomes with those obtained by the IOLMaster.
Methods
Medical records of 48 eyes from 48 patients who underwent uneventful phacoemulsification and IOL insertion were retrospectively reviewed. One of the two types of monofocal aspheric IOLs were implanted (Tecnis ZCB00 [n = 34] or CT Asphina 509M [n = 14]). Two different partial coherence interferometers measured and compared AL, keratometry (2.4 mm), anterior chamber depth, and IOL power calculations with SRK/T, Hoffer Q, Holladay2, and Haigis formulas. The difference between expected and actual final refractive error was compared as refractive mean error (ME), refractive mean absolute error (MAE), and median absolute error (MedAE).
Results
AL measured by the AL-Scan was shorter than that measured by the IOLMaster (p = 0.029). The IOL power of Tecnis did not differ between the four formulas; however, the Asphina measurement calculated using Hoffer Q for the AL-Scan was lower (0.28 diopters, p = 0.015) than that calculated by the IOLMaster. There were no statistically significant differences between the calculations by MAE and MedAE for the four formulas in either IOL. In SRK/T, ME in Tecnis-inserted eyes measured by AL-Scan showed a tendency toward myopia (p = 0.032).
As modern techniques in cataract surgery develop to control refractive outcomes with ever increasing accuracy, cataract surgery is now regarded as a form of refractive surgery [1]. Therefore, accurate measurements of ocular parameters and optimal formula selection are important for achieving better refractive results. The crucial ocular parameters for power calculation include axial length (AL), corneal keratometry (K) values, and anterior chamber depth (ACD) [2].
Since the introduction of the first optical biometer (IOLMaster; Carl Zeiss Meditec, Jena, Germany) in 1999, the IOLMaster is still considered the gold standard for AL measurement because of its accuracy and reproducibility [3]. The IOLMaster uses partial coherence interferometry (PCI), with a 780-nm laser diode infrared light for measuring AL [4]. Dual-beam PCI is applied to measure the length from the anterior surface of the cornea to the retinal pigment epithelium [5]. The K readings are calculated by analyzing the anterior corneal curvature at six reference points in a 2.5-mm-diameter optical zone. ACD is measured through lateral slit illumination [4].
In 2012, a novel optical biometer, AL-Scan (Nidek Co, Aichi, Japan), was introduced for clinical practice. AL-Scan uses an 830-nm infrared laser diode for AL measurement with a PCI [1]. K readings are measured using a double-ring keratometer, at two diameters (2.4 and 3.3 mm). The ACD is calculated using a rotating Scheimpflug camera. Compared to the IOLMaster, AL-Scan facilitates use by three-dimensional auto-tracking and auto-shot measurements [6].
It is essential to validate the accuracy of a newly adopted device by comparing it to the most commonly used instrument in clinical practice. There are few studies reporting the reliability of ocular measurement or IOL power prediction by AL-Scan compared to the IOLMaster [6,7]. To the best our knowledge, no data is available on assessment of IOL power calculations using four different formulas in two biometers. The aim of the present study was to compare ocular measurements by the AL-Scan biometer with those of the IOLMaster and to assess the accuracy of IOL power calculations by SRK/T, Hoffer Q, Holladay2, and Haigis formulas in patients who underwent phacoemulsification and implantation of one of two different types of intraocular lenses: Tecnis ZCB00 (AMO, Santa Ana, CA, USA) or CT Asphina 509M (Carl Zeiss Meditec).
The study protocol adhered to the tenets of the Declaration of Helsinki. This study was approved by the institutional review board of Seoul National University Hospital (1601-003-729) and the informed consent was waived. All patients referred to department of ophthalmology, Seoul National University Hospital, Korea, for cataract surgery between September 2014 and January 2015 were considered for inclusion in the present study. Detailed demographic data and the results of ophthalmologic examinations were retrospectively reviewed.
Only those subjects whose ALs were between 21 and 27 mm and who underwent uneventful cataract surgery were included. Subjects with any previous ophthalmic surgery or active ocular pathology, including zonular weakness or macula lesions, were excluded. Subjects with unobtainable ocular biometric values because of severe posterior capsular opacity were also excluded. The order of the instruments used for measurement was randomly determined for each patient. All examinations were carried out by a single experienced operator. Unreliable data, such as a signal-to-noise ratio less than 2.1 for either device, were excluded from the analysis [8].
A single experienced surgeon (MKK) performed all surgeries with a 2.7-mm-long, steep axis incision technique, and the IOL was implanted in the bag. One of the two types of monofocal aspheric IOLs was implanted. We chose the Tecnis ZCB00 IOL because it is one of the most commonly used one-piece IOLs with hydrophobic acrylic. CT Asphina 509M is a hydrophilic acrylic IOL treated with a hydrophobic coat with square edges. Thus, different material properties as well as the refractive index can affect the penetration of infrared light in each optical biometer. Therefore, we investigated the comparative efficacy of two biometers in each IOL. The expected refractive result was emmetropia or as close to emmetropia as possible, based on increments of IOL power. To compare postoperative predictability, the difference between expected refractive error and actual refractive error was compared between AL-Scan and IOLMaster groups. Refractive mean error (ME) was calculated as postoperative spherical equivalent minus predicted postoperative spherical equivalent, and refractive mean absolute error (MAE) and median absolute error (MedME) were defined as the average and median absolute value of the numeric error, respectively. These values were used to compare postoperative predictability. To evaluate agreement between formulas, the standard deviation and variance of ME values were used. The final refractions were performed four weeks after the cataract surgery.
In the IOLMaster device, predictions made using the SRK/T, Hoffer Q, Holladay2, and Haigis formulas were retrospectively optimized by adjusting a0, a1, and a2; personalized anterior chamber depth (pACD); surgeon factor (SF); and A constants. In the AL-Scan biometer, the constants were applied as follows in accordance with the manufacturer's recommendations: Tecnis - a0 = ŌłÆ1.177, a1 = 0.191, a2 = 0.248, pACD = 5.79, SF = 2.02, and A constant = 119.3; Asphina - a0 = 0.680, a1 = 0.400, a2 = 0.100, pACD = 4.90, SF = 1.12, and A constant = 117.9.
Statistical analyses were performed using PASW Statistics ver. 18.0 (SPSS Inc., Chicago, IL, USA). Paired t-tests were used to establish whether there was a significant systematic bias between the two devices. Bland-Altman plots were used to determine agreement between the two biometers [9]. The Wilcoxon signed-rank test was used to evaluate the differences in MAE, MedAE, and variance by the formulas for the two devices. Statistical significance was defined as a p-value <0.05 (two-tailed).
Forty-eight eyes of 48 patients (37 women, 11 men) were included in this study. The mean age of the patients was 69.04 ┬▒ 10.98 years (range, 43 to 87 years). Tecnis ZCB00 and CT Asphina 509M implants were placed in 34 and 14 eyes, respectively.
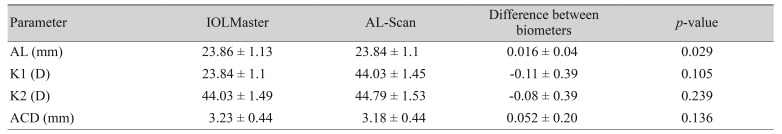
The mean difference in AL measurements between the two devices was 0.016 ┬▒ 0.04 mm, which was statistically significant (p = 0.029, paired t-test). The AL-Scan and IOLMaster provided a comparable mean K value of 2.4 mm. The mean difference was 0.11 ┬▒ 0.39 diopters (D) (K1) and 0.08 ┬▒ 0.39 D (K2), respectively. This value was not statistically significant (p = 0.105 and p = 0.239, paired t-test). The two biometers provided equal ACD measures, with a difference of 0.052 ┬▒ 0.20 mm (p = 0.136, paired t-test) (Table 1).
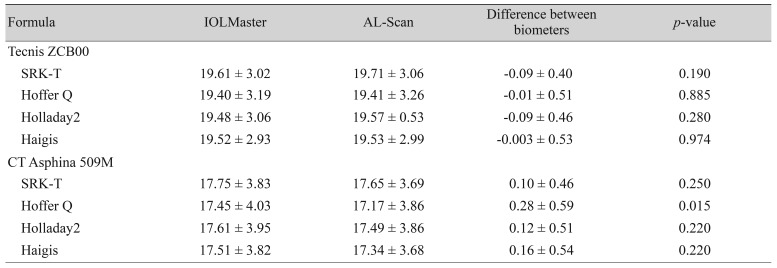
For the Tecnis IOL, the AL-Scan and IOLMaster provided comparable mean IOL power calculations for the four formulas. For the CT Asphina 509M, mean IOL power calculations by the SRK/T, Holladay2, and Haigis formulas were comparable between the two devices; however, when using the Hoffer Q formula, mean IOL power calculated by AL-Scan was lower than that calculated by IOLMaster. The difference between the calculations by the two devices was 0.28 ┬▒ 0.59 D (p = 0.015, paired t-test) (Table 2).
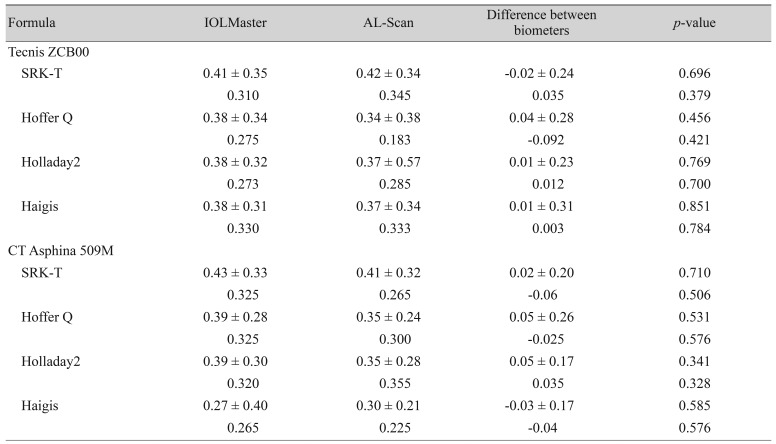
For the eyes implanted with a Tecnis ZCB00 IOL (34 eyes), there were no statistically significant differences for objective MAE and MedAE between the devices with the four formulas. Also, in eyes implanted with a CT Asphina 509M (14 eyes), the two devices showed comparable MAE and MedAE results for all four formulas (Wilcoxon signed rank test) (Table 3).
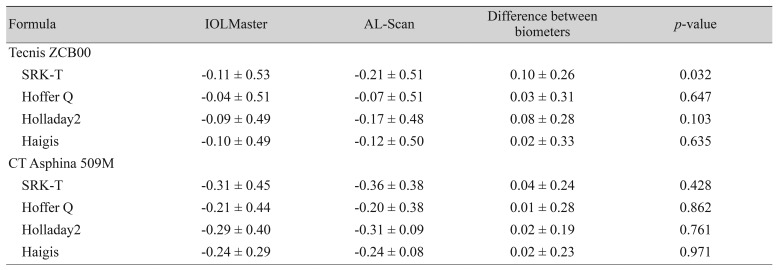
The ME values for Tecnis ZCB00-implanted eyes calculated using Hoffer Q, Holladay2, and Haigis formulas by the two devices were not statistically different. When using the SRK/T formula, the ME of Tecnis ZCB00-implanted eyes by AL-Scan tended to be myopic (p = 0.032, paired t-test). The ME measurements of CT Asphina 509M-implanted eyes were comparable among the four formulas (Table 4).
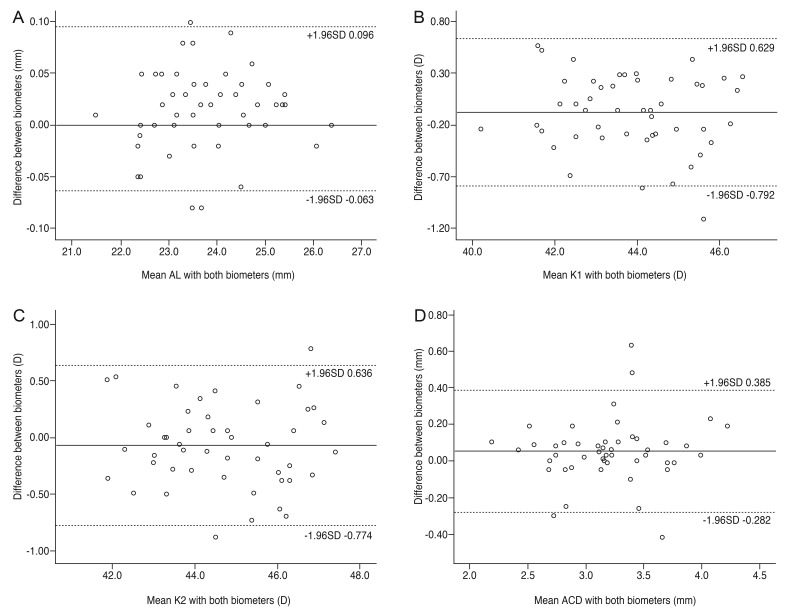
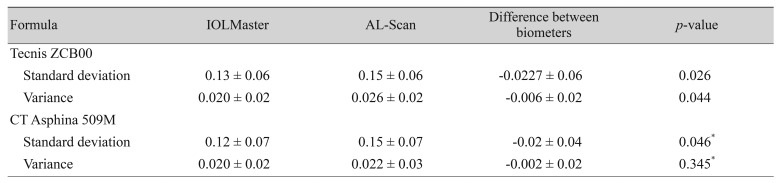
In Tecnis ZCB00-implanted eyes, the variance of ME calculations by the four formulas was higher for the AL-Scan than for the IOLMaster. The difference between devices was 0.023 ┬▒ 0.06 for standard deviation and 0.006 ┬▒ 0.02 for variance (p = 0.026 and p = 0.044, paired t-test). In CT Asphina 509M-implanted eyes, the two devices showed similar variance in ME calculations by the four formulas; however, the standard deviation for measurements by the four formulas using AL-Scan was greater (p = 0.046, Wilcoxon signed rank test) than that for measurements by the IOLMaster (Table 5). Fig. 1 shows the Bland-Altman plots and 95% limits of agreement between the two devices. Overall, the values of ocular parameters with the two devices showed high agreement and narrow 95% limits of agreement.
An accurate IOL power calculation is crucial for achieving satisfactory outcomes after cataract surgery. At present, optical biometry with the IOLMaster is considered the gold standard for AL measurements due to its good reproducibility and accuracy. The AL-Scan is a recently introduced optical biometer, and there were a few published studies that evaluated the both AL-Scan and IOLMaster. Huang et al. [6] and Kola et al. [10] demonstrated that ocular parameter measurements with the AL-Scan revealed excellent reliability and reproducibility. There were no statistically significant differences, and they showed narrow 95% limits of agreement for AL, ACD, and most K values between the two instruments. IOL power calculations using the SRK/T, Hoffer Q, Holladay2, and Haigis formulas revealed no significant differences between the AL-Scan and IOLMaster.
Kaswin et al. [7] also reported excellent correlations between the two devices for AL and ACD measurements and K readings. The IOL power calculations using the SRK/T and Haigis formulas were highly comparable between the devices. The MAE measures for 50 eyes implanted with either of the two hydrophobic, single-piece, monofocal, aspheric IOLs, the Acrysof SN60WF (Alcon Laboratories, Fort Worth, TX, USA) and the Tecnis ZCB00 (Abbott Medical Optics, Santa Ana, CA, USA), were statistically equivalent.
In the present study, the mean difference in AL measurements between the two devices was statistically significant (0.016 ┬▒ 0.04 mm, p = 0.029). In a previous study by Huang et al. [6], patients with severe advanced cataract were excluded based on the Lens Opacities Classification System III [11]. In contrast, we included patients irrespective of cataract grade, excluding only cases of dense posterior capsular opacity resulting in measurement failure with either one of the optical biometers. PCI measures axial eye lengths parallel to the vision axis as the patient fixates on the measurement beam or a coaxial fixation beam [5]. Thus, it is possible that outliers due to fixation problems in eyes with dense cataract led to the significant mean difference in AL between the two devices [12]. Even with correct alignment and accurate fixation, the measurement can be affected by the refractive index of the lens, which also varies with cataract grade. Severe nuclear cataract slightly increases the refractive index [13]. The IOLMaster and AL-Scan use different wavelengths of infrared light (780 and 830 nm, respectively), and longer wavelengths are able to penetrate tissue more deeply. Therefore, in addition to lens opacity, penetration depth can influence the measurement of AL [12,14]. The use of a longer wavelength resulted in a shorter measured optical distance [15]. Drexler et al. [5] demonstrated that AL measurement precision using PCI did not correlate with AL, but with cataract grade.
There was no positive or negative trend with either device, indicating that neither the IOLMaster nor the AL-Scan tends to overestimate or underestimate measurements in relation to the other device. In an average eye, a 0.10 mm error in AL is equivalent to an error of about 0.27 D in the spectacle plane [2]. Therefore, an average difference of 0.016 ┬▒ 0.04 mm was statistically significant, but it was too small to exert a significant effect on the final refractive outcome.
We assessed the accuracy of IOL power calculations using the SRK/T, Hoffer Q, Holladay2, and Haigis formulas in two different types of intraocular lenses: Tecnis ZCB00 and CT Asphina 509M. Even though AL measurements differed between the two devices, mean IOL power calculations using the SRK/T, Hoffer Q, Holladay2, and Haigis formulas were comparable for the Tecnis IOL. However, with the CT Asphina 509M IOL, the mean IOL power calculated by the AL-Scan using the Hoffer Q formula was lower than that calculated by the IOLMaster (0.28 ┬▒ 0.59, p = 0.015). Steep keratometric values can contribute to lower IOL power with the AL-Scan (mean average of K, 43.98 in IOLMaster vs. 44.41 in AL-Scan). In addition, the IOL power to achieve emmetropia is determined by the AL, K value, types of formulas that applied. Each formula estimates the effective lens position (ELP) in its own way. The SRK/T and Hoffer Q are two-variable formulas that rely on AL and central corneal power to predict the ELP. In the SRK/T formula, ACD is calculated using the Fedorov corneal height equation. On the other hand, the Hoffer Q formula applies a self-developed tangent curve to obtain the ACD. Additionally, the Haigis formula considers AL, K value, and also ACD when predicting ELP. The Holladay2 formula uses a white-to-white diameter in addition to the AL, K value, and ACD. As such, discrepancies in IOL power can be caused by the method used to predict ACD. Additionally, discrepancy in the IOL power calculations can be due to systematic errors in biometry, surgical technique, and the formulas [16]. The individual errors that arise between these multiple factors can cause a significant difference in power calculations for the CT Asphina 509M IOL, using the Hoffer Q formula.
MAEs and MedAEs for the two devices calculated using the four formulas were statistically equivalent. Although there was no statistical significance, the ME for Tecnis ZCB00 IOL tended to be lower with the AL-Scan. When using the SRK/T formula, the difference was 0.10 ┬▒ 0.26, which was statistically significant (p = 0.032). This difference could be caused by steep keratometric values (mean average of K, 43.98 in the IOLMaster vs. 44.41 in the AL-Scan). Considering that the SRK/T and Hoffer Q formulas are two-variable formulas, they appeared to be more affected by changes in keratometric values than the Haigis and Holladay2 formulas.
Less between-formula concurrence was observed in the AL-Scan. This suggests that the MEs estimated by the AL-Scan showed greater deviation and variance between the formulas compared with those by the IOLMaster. If the keratometric values or axial lengths were outside normal ranges, ŌĆ£between-formula concurrenceŌĆØ would be significantly reduced regardless of the type of biometer. Our study investigated the refractive outcomes using normal ranges of keratometric values and axial lengths to validate the accuracy of the measurement in each biometer. In other words, MEs with four different formulas (SRK/T, Hoffer Q, Holladay, and Haigis) were in significantly better agreement in the IOLMaster with normal ranges of keratometric values and axial lengths. This suggests that measurements in the IOLMaster can be more reliable than in the AL-Scan when subjects have normal keratometric values and axial lengths.
The primary goal of the current study was not to compare differences between the two IOLs, but rather to compare the results of the two biometers (IOLMaster vs. AL-Scan) in each IOL type. We wanted to determine whether the difference between the two biometry devices would be affected by the type of IOL. IOL power formulas use certain constants that are specific to each formula [17]. These constants adjust IOL predictions for systematic errors arising from the clinical environment. Thus, in order to improve accuracy, individual customization of these constants by analyzing larger postoperative data is important [17,18]. Individual customization of ŌĆ£A constantŌĆØ of the lens or refractive index can affect the clinical outcome depending on the type of IOL. In the present study, the measurement of the IOLMaster was previously optimized for both IOLs. However, the constants used for the AL-Scan were pre-optimized values, as we had not accumulated enough data for its optimization. Therefore, the current study was limited by the inability to directly compare outcomes between the two types of different IOLs. Further research with optimized constant values for the AL-Scan is warranted to obtain a more accurate comparison between the two biometers.
In conclusion, compared to the IOLMaster, the AL-Scan optical biometer provides highly accurate biometry data and IOL power calculations in patients with cataract. However, refractive outcomes obtained using the AL-Scan showed a tendency toward myopia and had less between-formula concurrence. These results suggest that the AL-Scan can be used in routine clinical practice for accurate biometry measurements, and further individual customization of constants would lead to better refractive outcomes.
Notes
Conflict of Interest: No potential conflict of interest relevant to this article was reported.
REFERENCES
1. Fontes BM, Fontes BM, Castro E. Intraocular lens power calculation by measuring axial length with partial optical coherence and ultrasonic biometry. Arq Bras Oftalmol 2011;74:166-170.


3. Shammas HJ, Chan S. Precision of biometry, keratometry, and refractive measurements with a partial coherence interferometry-keratometry device. J Cataract Refract Surg 2010;36:1474-1478.


4. Santodomingo-Rubido J, Mallen EA, Gilmartin B, Wolffsohn JS. A new non-contact optical device for ocular biometry. Br J Ophthalmol 2002;86:458-462.



5. Drexler W, Findl O, Menapace R, et al. Partial coherence interferometry: a novel approach to biometry in cataract surgery. Am J Ophthalmol 1998;126:524-534.


6. Huang J, Savini G, Li J, et al. Evaluation of a new optical biometry device for measurements of ocular components and its comparison with IOLMaster. Br J Ophthalmol 2014;98:1277-1281.


7. Kaswin G, Rousseau A, Mgarrech M, et al. Biometry and intraocular lens power calculation results with a new optical biometry device: comparison with the gold standard. J Cataract Refract Surg 2014;40:593-600.


8. Olsen T, Thorwest M. Calibration of axial length measurements with the Zeiss IOLMaster. J Cataract Refract Surg 2005;31:1345-1350.


9. Bland JM, Altman DG. Statistical methods for assessing agreement between two methods of clinical measurement. Lancet 1986;1:307-310.


10. Kola M, Duran H, Turk A, et al. Evaluation of the repeatability and the reproducibility of AL-Scan measurements obtained by residents. J Ophthalmol 2014;2014:739652.



11. Freeman G, Pesudovs K. The impact of cataract severity on measurement acquisition with the IOLMaster. Acta Ophthalmol Scand 2005;83:439-442.


12. Eleftheriadis H. IOLMaster biometry: refractive results of 100 consecutive cases. Br J Ophthalmol 2003;87:960-963.



13. Prinz A, Neumayer T, Buehl W, et al. Influence of severity of nuclear cataract on optical biometry. J Cataract Refract Surg 2006;32:1161-1165.


14. Faria-Ribeiro M, Lopes-Ferreira D, Lopez-Gil N, et al. Errors associated with IOLMaster biometry as a function of internal ocular dimensions. J Optom 2014;7:75-78.



15. Drexler W, Hitzenberger CK, Baumgartner A, et al. Investigation of dispersion effects in ocular media by multiple wavelength partial coherence interferometry. Exp Eye Res 1998;66:25-33.


16. Olsen T. Sources of error in intraocular lens power calculation. J Cataract Refract Surg 1992;18:125-129.


Fig.┬Ā1
Bland-Altman plots of biometric measurements from the AL-Scan and IOLMaster. (A) Mean axial length (AL), (B) mean keratometry 1 (K1), (C) mean K2, and (D) mean anterior chamber depth (ACD) with both biometers. D = diopters.
Table┬Ā3
Comparison of refractive mean absolute error and median absolute error between the two biometers
- TOOLS
-
METRICS

-
- 6 Crossref
- 0 Scopus
- 2,723 View
- 26 Download
- Related articles
-
Comparison of Accuracy of Six Modern Intraocular Lens Power Calculation Formulas2023 October;37(5)



 PDF Links
PDF Links PubReader
PubReader Full text via DOI
Full text via DOI Full text via PMC
Full text via PMC Download Citation
Download Citation Print
Print



