 |
 |
| Korean J Ophthalmol > Volume 33(3); 2019 > Article |
Dear Editor,
Schwannoma is a benign tumor which results from hyperplasia of myelin-producing Schwann cells. Its characteristics are ovoid shape, well circumscribed boundaries, and slow growth. These tumors usually occur in the head and neck regions, followed by the limbs and trunk. In the periocular area, the orbit is the most common site and accounts for 1 % of all orbital tumors [1]. Conjunctival schwannoma is extremely rare; to our knowledge only 13 cases have been reported in the literature and only one case has so far been published in Korea [2]. We report here a second case of schwannoma arising in the epibulbar conjunctiva.
A healthy 20-year-old man presented to our hospital with complaints of a subconjunctival mass which he accidently found on his left eye. His corrected visual acuities were 20 / 20 for both eyes and his ocular movement was not limited. There was no exophthalmos. On examination, the mass did not appear on simple dextro depression (Fig. 1A). However, when mild digital pressure was applied on this area, a 1.5-cm-sized rubbery, round, movable mass was pushed out up to the entire conjunctival fornix (Fig. 1B). On orbital magnetic resonance imaging, a homogenous orbital mass was found in the superolateral orbit adjacent to the lacrimal gland (Fig. 1C).
Surgical excision was performed through a superolateral conjunctival incision. The mass was located between the sclera and Tenon's capsule, and adhered to the sclera. The mass was carefully dissected off the sclera and removed. Histopathologic examination revealed a well-encapsulated tumor composed of spindle cells with Verocay bodies and sparsely arranged cells with myxoid stroma (Fig. 1D, 1E). There was no nuclear atypia. These findings were consistent with schwannoma.
Conjunctival schwannoma is a rare tumor which has an indolent clinical course. Of the 13 reported cases to date, our case has its own value as a second report in Korea [3]. Previously reported cases showed no sex predominance with seven being female and six male. Patient age ranged from 10 to 72 years. Among 13 reported conjunctival schwannoma, nine were epibulbar, two were palpebral, and one was in the forniceal area. As noted by Demirci et al. [4], since the bulbar conjunctiva is the most common site of conjunctival schwannomas, ŌĆśepibulbar schwannomaŌĆÖ was proposed to be a more descriptive term. Our case also involved the bulbar conjunctiva. Histopathologic features of conjunctival epibulbar schwannomas are not different from schwannomas in the rest of the body. Histopathologic findings in our case revealed whorls and a twisted configuration of spindle cells intermixed with haphazardly arranged elongated cells, which are consistent with schwannoma.
Treatment choice for conjunctiva schwannoma is complete surgical excision. This can be easily visualized and excised from adjacent tissue. Recurrence after complete excision is rare and to our knowledge, malignant transformation has not been reported in the conjunctiva. If scleral involvement due to the overlying lesion is suspicious, additional cryotherapy can be applied [4,5]. However, considering the benign pathology of the tumor itself, there seems no point in additional cryotherapy after complete excision. In our case, even though the mass adhered to the sclera, it was cleanly resected, thus there was no need to apply additional treatment and no recurrence was seen one year after surgery.
In summary, conjunctival epibulbar schwannoma is rare with very few cases are documented in the literature. Nevertheless, it should be considered and cannot be overlooked in the differential diagnosis of any subconjunctival nodular mass. Histopathologic examination can be helpful for diagnosis of conjunctival epibulbar schwannoma and complete excision is the curative treatment in most patients with rare recurrence rate.
Notes
Conflict of Interest: No potential conflict of interest relevant to this article was reported.
REFERENCES
1. Shields JA, Shields CL, Scartozzi R. Survey of 1264 patients with orbital tumors and simulating lesions: the 2002 Montgomery Lecture, part 1. Ophthalmology 2004;111:997-1008.


2. Kim SU, Gu MJ, Lee JK, Park DJ. A case of bulbar conjunctival schwannoma. J Korean Ophthalmol Soc 2009;50:1111-1114.

3. Grossniklaus HE, Green WR, Luckenbach M, Chan CC. Conjunctival lesions in adults: a clinical and histopathologic review. Cornea 1987;6:78-116.


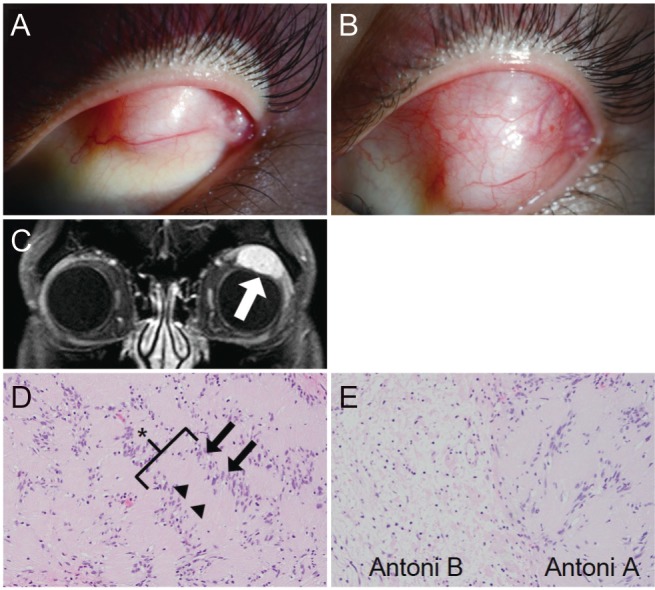
Fig.┬Ā1
Clinical and histological appearance of conjunctival epibulbar schwannoma. (A) Clinical photograph of the mass. On simple down gaze, the mass was barely seen. (B) When mild digital pressure applied on superotemporal area with same gaze, the whole mass was exposed. (C) On orbital magnetic resonance imaging of T1-weighted image, well circumscribed homogeneous mass (arrow) was found in the left superolateral orbit. (D,E) Histopathologic finding revealed alternating rows of densely palisaded elongated nuclei (arrows) and anuclear eosinophilic zones (arrowheads) composing Verocay bodies (asterisk) within Antoni A areas. Looser, less cellular Antoni B areas are found immediately adjacent. Informed consent was obtained from the patient for publication of this case report and any accompanying images.
- TOOLS
-
METRICS

-
- 2 Crossref
- 0 Scopus
- 1,842 View
- 18 Download
- Related articles



 PDF Links
PDF Links PubReader
PubReader Full text via DOI
Full text via DOI Full text via PMC
Full text via PMC Download Citation
Download Citation Print
Print



